|
|
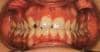
Figures 1 (top) and 2 (bottom) demonstrate the typical results when the new mechanotherapy is used to treat an open bite. |
By Jack C. Fisher, DMD, and Jay B. Burton, DMD, MBA
Open bites have long been the most difficult type of malocclusion to treat and retain. The etiology is multifactorial, including: inheritance, allergies, mouth breathing, low tongue position, forward tongue position, constricted upper arch, super erupted molars, reverse swallowing habit, trauma, idiopathic condylar resorption, etc. The relationship between these factors makes it difficult to diagnose with 100% accuracy. Regardless of the etiology, we as orthodontists are responsible for treatment of open bite patients when they present to our practices.
New Modalities
In the 1980s and early ’90s, many open bite cases were treated with fixed orthodontic appliances and orthognathic surgery. During this time, most insurance companies covered this treatment modality. Unfortunately, getting approval from insurance companies for this type of treatment has become difficult, if not impossible. This has left the profession of orthodontics with the challenge of developing alternative treatment modalities to correct this malocclusion.
However, we cannot discuss new modalities of open bite treatment without first addressing the past stability of surgical treatment. With regard to the stability of surgical treatment, Espeland et al wrote that “surgical impaction of the posterior maxilla ?2 mm relapsed on average by 31% and inferior repositioning of the anterior maxilla ?2 mm relapsed by 62%.”1 If a treatment modality to close open bites, without surgery, falls within these envelopes of relapse, we can conclude that this new modality is an acceptable alternative to surgical intervention. Proffit et al states:
Successful treatment of skeletal open bite during growth requires control of downward growth of the maxilla and eruption of posterior teeth so that mandibular rotation is prevented. This can be extremely difficult to accomplish. Continued vertical growth in the late teens is a major problem that often occurs after orthodontic treatment has been completed. After excessive vertical growth has occurred, there are only two approaches to treatment of open bite: elongate the anterior teeth, which leaves the skeletal component of the deformity uncorrected, or depress the posterior teeth.
If an appropriate force system could be developed and applied, it would be possible to intrude posterior teeth. Bite blocks between the posterior teeth, with or without magnets, can prevent further eruption, but significant intrusion in adolescents or adults is difficult to document and rarely if ever achieved. Open bite can be corrected in patients who are beyond the adolescent growth spurt with multiloop edgewise technique, but the major effect is extrusion of anterior teeth rather than ?intrusion posteriorly. Once excessive vertical development has occurred, orthognathic surgery is the only way to correct the jaw rotations and reduce anterior face height.2
With this in mind, this article offers a treatment modality that meets the objectives stated by Proffit et al and falls within the surgical relapse rates regarding treatment stability. Looking at Figures 1 and 2, we see a typical result when using the mechanotherapy described below.
Use of TSADs

Each spring produces about 225 g of force. Using four springs, two per side, yields the resultant vertical force of around 800 g total. Additionally, it is important to incorporate an intrusive force on the lower posterior segments in cases that exhibit a lower reverse curve of spee that is the result of supra erupted posterior teeth. The lower appliance uses two to four TSADs for intrusion (Figure 5). The TSADs are placed between the first and second molars and/or mesial to the first molars (Figure 6).

Force Systems
When these two appliances are combined to close an open bite, there are four active force systems:
- An acrylic button on the upper appliance is placed approximately 5 mm off of the palate. This provides an intermittent vertical force every time the patient swallows.
- Bite blocks on the upper appliance are constructed so that the only teeth contacting the appliance initially are the second molars. As the posterior teeth intrude, the first molars and the bicuspids begin to contact.
- A maxillary appliance attached to springs provides a vertical force.
- A mandibular appliance attached to springs provides a vertical force.
Results

When 3 mm of upper and lower intrusion is achieved (a total of 6 mm intrusion), this results in the potential closure of an 18-mm open bite and the Y-axis can close as much as 5º. Because of the amount of intrusion and rotation of the mandible, the canines often begin to occlude too soon due to the autorotation. In order to continue the posterior intrusion, it is often necessary to employ finger springs on the maxillary appliance to push the canines buccally during intrusion, as seen in Figure 3.

We have found that 5 months of wearing the appliances is usually sufficient time to close most open bites. In severe cases, the appliance can remain active for 6 months. Upon removal of the maxillary ?appliance, there is usually a posterior open bite, which is normal at this stage in the treatment protocol. Usually, some relapse is warranted because of the posterior open bite that has been created (Figure 7). The lower appliance is not removed so as to continue to take advantage of the tongue spurs placed on the lower appliance.

The patient is then instructed to return to the clinic in 4 weeks to place the fixed brackets, which are placed in an open bite position. If needed, the TSADs, which have been left in on purpose, can be used as vertical control by ligating the first molars to the TSADs. This should prevent any unwanted relapse.
As with any open bite case, retention is a major concern. We recommend an upper wrap-around type of retainer and a lower Hawley retainer with posterior bite blocks (2 to 3 mm) and tongue spurs (Figure 8).

Before attempting this mechanotherapy, it is recommended that the clinician become proficient in the placement of infrazygomatic TSADs in order to obtain consistent results. The best education to gain this competency is to first become proficient in placing these TSADs on fresh tissue specimens during a training course. This appliance meets the objectives reported in the footnoted article to close open bites.
While long-term follow-up studies are needed to compare the stability of this technique with that found in orthognathic surgical closure, the preliminary results we have observed are positive and encouraging. OP
 |
Jack C. Fisher, DMD, has maintained a private practice since 1982. He can be reached at [email protected]. Jay B. Burton, DMD, MBA, is an orthodontic resident at New York University. He can be reached at [email protected]. |
References:
- Espeland L, Dowling PA, Mobarak KA, Stenvik A. Three-year stability of open-bite correction by 1-piece maxillary osteotomy. Am J Orthod Dentofacial Orthop. 2008;134(1):60-66.
- Profitt WR, Bailey TJ, Phillips C, Turvey TA. Long-term stability of surgical open-bite correction by Le Fort I Osteotomy. Angle Orthod. 2000;70(2):112-117.