By Jack Fisher, DMD, and Jay Burton, DMD, MBA
As the use of temporary skeletal anchorage devices (TSADs) has become more prevalent, novel approaches to space closure have become more prevalent as well. With new approaches come new benefits and new complications. Unfortunately, a lot of orthodontic literature focuses on the success that comes with using TSADs, but minimizes or simply does not mention complications associated with their use.
One area where TSADs have been useful is space closure. This article will primarily focus on the protraction of posterior teeth using TSADs, as well as the potential complications that can arise using different methods of biomechanics.
Considerations When Closing Space

Skeletal anchorage can eliminate or minimize the aforementioned complications. However, using TSADs necessitates a good understanding of biomechanics if you are to avoid potential complications. When using TSADs, either as direct or indirect anchorage, you must consider the effects a force has in all three planes of space. You consider not only the tooth or teeth being protracted, but also the other teeth in the system if you are using indirect anchorage.
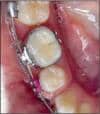
From an occlusal perspective, the center of resistance for a lower molar is pretty close to the center of the crown. If a TSAD is placed at some point anterior to the molar and a protraction force is applied from the molar to the TSAD, the molar will tend to rotate around its center of resistance. The further away from the center of resistance the force is applied, the greater the resultant moment. Depending on the stiffness and shape of the archwire, a tremendous amount of friction can be created during protraction (Figure 1).
Friction

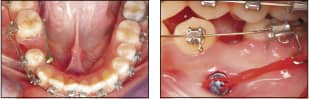
Another option is to attach power thread on the lingual and route the power thread around the mesial of the molar, then attach the power thread to the wire that is running through the buccal tube of the molar (Figure 4).
A third option (Figure 5) is to ligate the anteriors with a common tie, then place the power thread to the lingual of the premolar and attach the other end mesial to the cuspid to the archwire being used. The adverse effect from this particular technique could be the reclination of the anteriors.

Vectors of Force
A second complication that needs to be addressed when using TSADs is the vector of force from the TSAD to the molar as viewed from the buccal or lingual. Many companies tend to oversimplify the mechanics needed to protract the molar by illustrating the force from the TSAD directly to the molar hook.
Anchor Design and Placement
The design and placement of a TSAD have a direct effect on the amount and direction of force application. Four types of TSADs can be used for the type of mechanics we have discussed. These include the following:
1) Miniscrew pins: These screws are simple pins with threads that can be placed unicortically or bicortically. When placed bicortically, they tend to be more stable than those placed through only one cortical plate.
2) A screw with a base or a platform designed to be inserted to the point where the base is contacting the cortical bone. This design has more of a “bone plate effect,” resulting in increased stability as compared to a simple pin-type TSAD.
3) The transcortical type. This is the most stable type because it transverses both cortical plates completely.
4) Bone plates that have two to four screws holding the plate in place. The screws need to be at least 4 mm in length to yield a more stable TSAD than the screws with the platform seated on cortical bone. For protraction, bone plates can be placed either mesial or distal to the canines. More research needs to be conducted with these devices, specifically with regard to stability versus the other types of TSADs. A potential issue for patients regarding the bone plates is the additional cost of the device and the expense of placement.
The area of placement of TSADs is a common concern. The most common mistake clinicians make when placing the “pin type” and TSADs that have a base is to place them too close to the crest of the alveolus. This can result in fracture of the alveolar crest upon insertion. Also, the cortical bone becomes thinner as one moves toward the crest of the ridge, thereby potentially creating a less stable situation. TSADs should be placed approximately at the estimated level of the center of resistance of the first molar (about the level of the furcation). This will allow for horizontal force application through the center of resistance, thereby translating—instead of just tipping—the molar.
Tissue Overgrowth

Open Bites
When you are protracting the first and second molars, the second molar should be bracketed and leveled before the protraction of the first molar is initiated. If you don’t do this, and the first molar crown tips mesially, you could create a unilateral open bite. The wire in this case should be a round stainless steel wire of sufficient stiffness to prevent the aforementioned tipping. The round wire will have less friction, which will place less stress on the TSAD and increase the rate of closure.
A final complication that can occur when you are closing spaces in the lower arch using skeletal anchorage deals with the coefficient of friction as posterior teeth move mesially on the wire. If you use a continuous archwire and ligate the anterior teeth to the archwire, the lower anterior teeth may flare during the space closure if the molar tube binds on the wire.
When you are closing space unilaterally and this happens, this coefficient of friction can create a unilateral anterior open bite (Figure 9). If the patient has a deep bite with an unacceptable amount of overjet, the friction created on the archwire by the posterior teeth moving mesially could be considered positive sequelae. If you don’t want anterior tooth movement, then do not ligate the anterior teeth during the posterior space closure and apply a protraction force on the lingual of the molar. This will help minimize the rotation and binding that can occur. Also, you could use segmental mechanics as opposed to a continuous archwire.
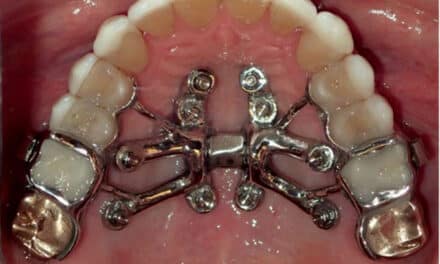
A Molar Protraction Appliance
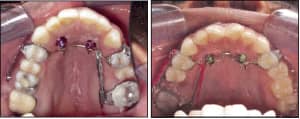
1) Solder a small hook to the bar approximately 4 mm from the band on the side that needs space closure.
2) Solder a buccal tube to the molar band on the buccal, then solder a tube on the palatal aspect of the same band at a level approximating the center of resistance of the molar being protracted.
3) Solder a .032 round stainless steel wire to the transpalatal bar and extend it through the tube soldered to the palatal of the molar band.
4) Solder another .032 round stainless steel wire to the buccal aspect of the bicuspid band, and extend it through the tube that you soldered to the molar band.
5) Place two TSADs anterior to the transpalatal bar and ligate them to the bar.
6) Place power chain from the hook soldered to the transpalatal bar to the round wire, extending through the tube on the palatal. Also attach the power chain to the buccal aspect in the same manner. The molar will translate, closing the space. This can be accomplished prior to bracketing the case.
Osteoperforations

Conclusion
Closing spaces using TSADs has often been presented as simple and easy, with few or no side effects. There have been a number of advertisements published in journals that simply illustrate placing the device anterior to the tooth/teeth that need to be protracted, with a force placed from the skeletal anchorage device to the tooth/teeth—and the space miraculously closes without any complications. We hope this article has pointed out some of the potential complications and solutions related to space closure with TSADs.
Jack C. Fisher, DMD, has maintained a private practice since 1982. He can be reached at [email protected].
Jay Burton, DMD, MBA, is an orthodontic resident at New York University. He can be reached at [email protected].