By Alison Werner | Photography by Dave Trumpie
Louis G. Chmura’s wife of 24 years, Penny, often used to say it was a comfort to hear her husband snore at night. It reassured her that he was there. What she and Chmura, DDS, MS, didn’t know was how unreassuring his snoring should have been.
According to the National Sleep Foundation, more than 18 million American adults suffer from sleep apnea, or obstructive sleep apnea (OSA). These patients experience periods in which their breathing is briefly and repeatedly interrupted during sleep. These interruptions, or pauses in breathing, can last anywhere from a few seconds to minutes and may occur 30 or more times an hour. When breathing restarts, it is often with a loud snort or choking sound.
OSA occurs when the muscles in the back of the throat fail to keep the airway open. The airway can be obstructed by the tongue, the tonsils, and/or adenoids, which prevent air from flowing. Not only does it cause poor sleep quality, it also causes low blood oxygen levels. As a result, people with sleep apnea often experience a number of comorbidities, including hypertension, heart disease, and mood and memory problems.
Chmura’s introduction to sleep apnea came in the 1980s, when he and his future wife, Penny, worked midnights at a Lansing, Mich, hospital—he as an orderly and she as a nurse. There, Chmura’s job was to turn coma patients every 2 hours during the night, then sit by one particular patient’s bed.
“It was really quite comical,” Chmura recalls. “He would breathe for a while, then stop. So I would poke him. He would swear and resume breathing, but I would have to again poke him every few minutes all night long.” What Chmura didn’t realize until 2 decades later was that this was sleep apnea, and he was helping to keep this patient alive.
[sidebar float=”right” width=”225″]Practice Profile: Chmura Orthodontics
Locations: Marshall, Battle Creek, and Lansing, Mich
Average patients per day: 50 to 70
Number of chairs per location: Six, five, and four, respectively
Office square footage: 3,996, 2,500, and 1,500 square feet, respectively
Years in practice: 27
Days worked per week: 3 to 4
Education: BA Chemistry, Michigan State University, 1978; DDS, University of Michigan, 1985; MS, Orthodontics, University of Michigan, 1987
Top 4 products used: Suresmile, ICAT, Invisalign, Dolphin 3D & Management
Website: teamchmura.com; chmuraortho.com[/sidebar]
In high school, Chmura was in good shape. He remembers playing basketball all morning, tennis all afternoon, then running a 5-minute mile to make sure he kept in shape. Then came college. While he still played basketball and tennis, he fell victim to the “freshman 15.” Then about 10 years ago he tore his Achilles playing basketball, and his active lifestyle came to a halt. With the resulting weight gain, his history of snoring became a huge concern.
During the long recovery from his injury, Chmura slipped into a more sedentary lifestyle. With the inactivity, he felt more exhausted than ever. In addition, he could tell his health was declining. Meanwhile, his wife suddenly found herself staying up all night and poking Chmura when his breathing stopped. The snoring was no longer the comfort it had once been.
Chmura was on a downward spiral, and he feared he wasn’t going to survive it. He sought help. The diagnosis: sleep apnea.
The Achilles injury and the resulting lifestyle change had been the trigger. “I had compensated for my airway anatomy for a long time, and suddenly I stopped the activity that had kept sleep apnea at bay. As a result, I got sicker and sicker,” he says.
To help those who don’t understand how debilitating sleep apnea can be, Chmura likens it to a college finals week—except this one has no end. “You know how you get to finals week, you’re cramming and you end up sleep-deprived. At the end of the week, you breathe a sigh of relief and say it’s over. But in the days that follow, you get sick and catch up on sleep. Imagine a finals week every week, and you never catch up. You’re chronically tired. You sleep, but you never get deep sleep.”
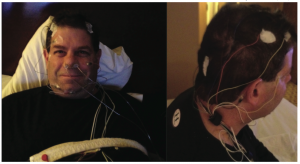
Here, Lou Chmura, DDS, MS, undergoes a polysomnogram to diagnose his obstructive sleep apnea. Photo Courtesy of Lou Chmura, DDS, MS
Upon diagnosis in 2005, Chmura was fitted with a CPAP machine. For adults with moderate to severe sleep apnea, CPAP is the most common form of treatment. Consisting of a mask fitted over the mouth and nose during sleep, the machine blows air into the throat. The pressure from the air helps keep the airway open.
Like many CPAP users, Chmura found the experience miserable. However, he got some relief, so he stuck with the treatment. In fact, he didn’t realize how much of an impact the device was having until he was traveling and his luggage, in which the CPAP was packed, was lost. “I had 2 days of misery,” he recalls. “I realized at that point that this really did make a difference.” The problem, however, was that Chmura’s health was still declining, just not as fast with CPAP.
Chmura switched into research mode and began looking into sleep apnea, with the hope of finding alternative treatments that would save his life. What he found was how common sleep apnea is.
The American Sleep Apnea Association estimates that sleep apnea is as common as type 2 diabetes. Yet, many sleep apnea sufferers remain undiagnosed and untreated due to a lack of awareness by patients and healthcare professionals. While 18 million adults are currently diagnosed with OSA, it’s believed that the number could actually be closer to 30 million due to underdiagnosis.
Chmura’s research told him some of what he already knew: CPAP is considered the “gold standard” treatment for sleep apnea, even though patient compliance is a chronic problem—with estimates that as few as 50% of people who are prescribed CPAP actually use it regularly. Another common treatment is uvulopalatopharyngoplasty, or UPPP, which removes excess tissue in the throat to widen the airway. However, with a success rate of 30% to 50%, Chmura wasn’t convinced this was the right choice for him. Instead, he opted for maxillomandibular advancement surgery.
In his research, Chmura discovered another treatment option that spoke to him as an orthodontist: oral appliances. At that moment, he realized that his personal experience with sleep apnea and his training as an orthodontist could help others, including his own patients. Since then, Chmura has been a champion of the role orthodontists can play in treating sleep apnea.
Finding a Pathway
Chmura’s path to orthodontics wasn’t a straight one. He came to orthodontics by way of a brief career in engineering. While engineering appealed to his methodical way of thinking, it lacked the opportunity to work with people and help improve their lives. Eventually, Chmura found himself choosing dentistry over medicine, then focusing on orthodontics. He appreciated the diversity and complexity the field of orthodontics could offer in treating patients.
Since completing his Master’s in orthodontics at the University of Michigan in 1987 and practicing first in Virginia and then in Marshall, Mich, Chmura has looked for ways to innovate his practice. It started with using lasers for gingival aesthetics before progressing to TADs and 3D imaging. With the adoption of each new technology, Chmura has approached the process with an engineer’s mind, carefully laying out a plan for educating himself and then incorporating what he’s learned step-by-step. His expertise has in turn led to opportunities to lecture.
When Chmura realized orthodontists could play a role in treating sleep apnea, he took the same methodical approach to make himself an expert, taking numerous courses on sleep apnea by a number of experts in the field before synthesizing the information so that it best applied to what he could do as an orthodontist. Fast forward to 2012, when Chmura was approached by Henry Schein Orthodontics to join a task force to determine the roles orthodontists could play in treating sleep apnea. Dave Paquette, DDS, MS, MSD, was already part of the task force and wanted Chmura to join and bring his sleep expertise.

Unfortunately, Chmura and his staff realized they were overtaxed. “We had just incorporated 3D and TADs 2 years before this, and had just started SureSmile. Each one of these has a tremendous learning curve,” he says. A member of his team suggested they cut something, and Chmura realized she was right. Something had to go.
Despite the clinical success with sleep apnea, it had become a burden for the practice. Chmura found himself spending more time with the sleep patients in the new patient exam, explaining the disease and what solutions he could offer, but these patients more often than not were focused on what insurance would cover, which was little to nothing.
Chmura was understandably frustrated. “I would look at them incredulously because this was their health, and they wanted to know what insurance would pay,” he says. In fact, his local sleep doctor was thrown by Chmura’s decision. “What do you mean?” Chmura remembers the doctor asking. “When I send them to you, I know it’s OK. I don’t have to worry about [these patients] anymore, because you’ve got it handled.” But Chmura had no choice. “I couldn’t afford it.”
So when Henry Schein Orthodontics and Paquette came knocking 6 years later, he was honest. “I told them, I couldn’t pull this off on my own. I had purchased six ApneaLink™ [home sleep testing devices] at $2,200 a piece. I was going to test every patient before and after different kinds of ortho treatment. This was my money, and I couldn’t make it happen,” he remembers.
But when he stopped to think about it, Chmura realized he ran out of steam because it was all on him to make it work. Now he had the opportunity to not only have corporate financial backing, but also the opportunity to work with people like Paquette; Nelson Diers, DDS, MS; Bill Thomas, DDS, MS; Ron Redmond, DDS, MS; Terry Carlyle, DDS, MSc, FRCDC; Paul Damon, DDS; and JC Quintero, DMD, MS—all members of the task force that was being put together.
“Working with these incredibly gifted and innovative people from around the country, I thought, even if all we got really good at was making oral appliances, and that’s all I thought we could do, I realized we could make this happen,” he says. “We had the resources to make this a viable thing and to figure out a way to bill insurance and get paid.”
The team began to educate themselves with a literature review, reading everything they could get their hands on that applied to sleep apnea, attending the American Academy of Dental Sleep Medicine meeting and numerous other sleep courses. One thing they learned was that sleep apnea treatment could also apply to the adolescent population.
“Whoa! Wait a second,” Chmura found himself saying. “What did you say? Sleep apnea in kids? I had no idea.” Studies show that the prevalence of childhood sleep apnea ranges from 2% to 3% to as high as 10% to 20% in habitually snoring children, according to the National Sleep Foundation. Chmura had only been treating adults for OSA in his practice, but as part of the task force, he was coming across numerous published articles showing that, in addition to removing tonsils and adenoids, rapid palatal expansion has a very positive effect on reducing sleep apnea in children.
“As orthodontists, we could prevent kids from getting sleep apnea or we could cure kids who have sleep apnea because we can change the anatomy. Dave [Paquette] and I, at least, had no idea [before reading that literature] that we could do that,” Chmura says.
The task force expanded Chmura’s perspective on the role orthodontics could play in treating sleep apnea sufferers and in giving them alternatives to CPAP or oral appliances, both of which only work if the patient actually uses them. “In orthodontics, we have the potential for changing the anatomy in such a way that we take away the sleep apnea forever. That’s a game changer,” Chmura says. Furthermore, an “airway-friendly” approach to orthodontic treatment shows promise for helping adults with sleep apnea as well.
The task force created a systematic orthodontic approach to treating sleep apnea that covers everything from screening and testing to obtaining a diagnosis and performing treatment. To ensure practices have long-term success implementing sleep apnea treatment, they included components addressing billing and insurance, referral development, and patient education and marketing. The task force combined all of this into a 2-day course led by Chmura and Paquette that is now presented across the country.
Since joining the task force, Chmura has once again started treating sleep apnea in his practice. He screens every patient who comes in—both adults and children. The practice altered its health history—asking, for example, whether or not a patient snores, are they a heavy breather, do they sweat when they are asleep, etc—and Chmura has changed how he views questions he already was asking—such as history of cardiac disease, diabetes, high blood pressure, for example. These can all be signs that there is a sleep problem.
In addition to the changes to the health history, every adult patient fills out the Epworth Sleepiness Scale and a sleep partner questionnaire. Parents of every child are asked to complete a pediatric sleep questionnaire.
Chmura has also enhanced his clinical exam. “For example, we always thought that when kids
ground their teeth that there was an occlusal interference. Well, when I found out that bruxism—which is grinding your teeth—is part of sleep apnea, we started looking at that. I also started looking at tonsils. I never paid attention to them before—I looked, but I wasn’t focused. I know now that it doesn’t matter how well I treat a case orthodontically; if I don’t handle the airway, it will fail,” Chmura says. “A lot of the signs and symptoms that we always looked for are still there; they just mean things that are different now.”
But Chmura cautions that he’s not diagnosing sleep apnea. He may send a patient who he suspects of having sleep apnea home with a home sleep test, but he then turns those results and his findings over to a sleep doctor for a diagnosis. Still, Chmura is getting pretty adept at identifying sleep apnea. “By the time we send them to a sleep doctor, [they’re] usually looking over the data and rubber stamping it. [They’re] often ruling out the one or two things it could be otherwise.”
And as for building those relationships with sleep doctors, Chmura admits it’s a bit of an uphill battle. Not only do you need to be able to talk the talk and show that you know sleep medicine, “You have to show them what you are doing and why you are doing it,” Chmura says. That can include educating sleep doctors on why an oral appliance isn’t the only solution to CPAP noncompliance.
On the other hand, “If they opt for an oral appliance, it’s easier to fit an oral appliance when the teeth are straight. To fit it to crooked teeth is very difficult. The other part is, once we align teeth, so long as we do something to hold them there, they stay aligned. So our solutions are more permanent than just putting in your oral appliance.” Still, Chmura knows it’s going to take some time, more patients, and more documentation before sleep doctors will say, “That’s right. Let’s think about orthodontics for this one.”
This time around, Chmura is committed to keeping the sleep apnea component of his practice going. With statistics showing that the 18-year survival rate drops 40% for patients with untreated sleep apnea, he knows that orthodontic treatment done properly can do much more than straighten teeth. It can save lives.
“Straightening teeth is a wonderful thing to do; don’t get me wrong,” Chmura says. “But at the end of the day, if that was all you did [in your career], that would be pretty hollow to me. What’s really cool is we can not only give people great smiles and good bites, but within that scheme, we can give a [father] the opportunity to walk [his] daughter down the aisle.” OP
Alison Werner is editor of Orthodontic Products. She can be reached at [email protected].












