by Straty Righellis, DDS
The oops! and ahs! of interdisciplinary care

In the case of a missing upper lateral incisor, the orthodontist either opened a space to prosthetically replace the missing upper lateral incisor, or closed the space and substituted an upper cuspid for the missing upper lateral incisor. If space was opened for a bridge, the orthodontist’s concern was simply to provide the restorative dentist with relative root parallelism for “line draw” in bridge preparation and a space for a lateral pontic. The restorative dentists were quite adept at making most bridge-abutment positions workable, but the size and shape of the lateral incisor pontic and associated gingival contours were limited to existing space and the alveolar ridge that was available.
In the case of transforming a substituted upper cuspid into a “lateral incisor,” the orthodontist asked the restorative dentist to “lateralize” the cuspid as necessary for optimal aesthetics. The restorative dentist modified the clinical height and width of the substituted upper cuspid by reshaping the cusp tip, by adding composite material to round out the flat cuspid line angles, and by reducing the usually bulbous labial contour.
Missing posterior teeth treatments were primarily uprighting the posterior teeth about their apices for bridge placement. Most posterior teeth were tipped into the long-standing extraction sites, and the resultant edentulous alveolar ridge was often too narrow buccal-lingually to safely move the larger molars into the narrow edentulous area.
Technology and Collaboration
While the diagnostic criteria for treatment-planning for a patient with missing permanent teeth has not changed remarkably over the years, the diagnostic data gathered is more involved and our treatment solutions are more sophisticated.
The orthodontist still evaluates the malocclusion and facial balance to determine the feasibility of the two treatment options, but recently, advances in periodontal diagnosis and surgical techniques, improvements in composite and porcelain dental materials, and advances in dental-implant designs have given the team numerous treatment options to improve the color and shape of the teeth, and also to enhance the supporting bone and soft tissue.
With these increased options, the need for enhanced communication in diagnosis and treatment planning is critical. With clear communication among the various dentists, we can achieve optimal results with fewer “oops!” and more “ahs!”
Common Treatment Goals
Interdisciplinary care has seven main treatment goals:
1) satisfaction of the patient’s chief complaint;
2) optimum dental aesthetics;
3) optimum facial aesthetics;
4) functional occlusion;
5) dental stability;
6) improvement of periodontal health; and
7) improvement of TMJ health.
While the treatment goals are listed in seven separate categories, they are interrelated; and satisfying one treatment goal requires satisfying all goals. If a treatment goal is not satisfied, it must be documented and listed as a treatment limitation.
The team members—the orthodontist, periodontist, restorative dentist, and oral surgeon—must not only agree that these goals are important for predictable, optimal treatment outcomes, but also must have measurable criteria by which to measure their achievement of each goal. Space limits discussing the measurable criteria for each goal, but it is critical that each team member understand what is required to meet these goals and produce the treatment outcome.
The team must be aware of technological advances and know what questions to ask the other team members to ascertain their information level.
Diagnostic Data
A complete oral exam, including TMJ analysis with mounted diagnostic casts in centric relation, identifies the nature of the malocclusion with the jaws centered in the fossae to analyze how to achieve the functional occlusion and TMJ treatment goals. Prior to any dental treatment, the team must be confident that the TMJ status is stable with the jaws centered in their most repeatable position—specifically, centric relation. Some dentists also use the term “seated, stable condylar position.” If this position is not identified prior to prolonged orthodontic treatment, it may be uncovered during or after treatment, possibly changing the outcome of the functional occlusion.
Cephalometric and facial photographs address facial balance and dental aesthetic treatment goals. Full-mouth x-rays and a periodontal report evaluate the periodontal treatment goal. Addressing the chief complaint is important, but often can change as the patient gathers more information about his or her dental problems and what dentistry has to offer. Questions about the patient’s chief complaint should be asked at the initial examination, but also at the final pretreatment consultation, after all information has been gathered.
Bumps in the Road
While completed interdisciplinary cases are gratifying, there are bumps along the road to treatment. Many of those road bumps are resolved in advance by communicating with your team and knowing what each specialist can do. This article is designed to provide a framework in which to share some of the issues I have experienced, in hopes of minimizing road bumps on your next trip to optimal patient satisfaction and treatment outcome.
I will limit my discussion to “orthodontics and dental implants” and “orthodontics and gingival symmetry.” I will subdivide dental implants into “dental implants after orthodontic treatment,” “dental implants prior to orthodontics for anchorage use,” and “final implant position.”
Orthodontics and gingival symmetry will be limited to two areas: 1) cuspids substitution and gingival symmetry, and 2) orthodontics prior to veneer placement.
Dental Implants Placed After Orthodontic Treatment
If space can be obtained, is the alveolar process adequate, in both buccal-lingual and occlusal-gingival dimensions, for the dental implant? In cases where no alveolar graft is used, the dentist is required to compensate by placing a more labially positioned crown. Using alveolar grafting, on the other hand, allows for proper crown placement.
If there are missing anterior teeth, what is the relationship of the anticipated pontic’s gingival margin when the patient is smiling? How much gingival margin will show, and what steps are needed to maximize the dental aesthetics of the finished crown? What will the resultant gingival papillae look like?
To resolve these diagnostic issues, the team must agree on the dental and facial aesthetic goals. They must be able to visualize the finished result.
During treatment, the orthodontist must be aware of the angulation of the teeth adjacent to the missing teeth. With preadjusted brackets, awareness of built-in bracket angulation is critical to avoid overtipping the root of the teeth mesial to the missing tooth.
Often, it is advisable to separate the root apices more than usual prior to implant placement. Each dentist has a different “comfort zone” when it comes to dental-implant placement.
You can save valuable treatment time by bracketing these teeth in anticipation of root angulation and implant location. After implant placement, the teeth can be rebracketed more ideally to provide ideal angulations of the adjacent roots to satisfy the dental aesthetic treatment goal of the interdisciplinary team.
Decisions about bone and soft-tissue grafts should be discussed prior to appliance placement. The dentist may request tomograms or CT scans of the implant sites to view the quality and quantity of the bone to help make decisions on grafting and dental-implant placement. If hopeless teeth are planned for extraction, the site is a possible donor site.
In our adult patients, the execution of our treatment plans often can be made without much interruption. However, in the growing patient, the variability of continued dental alveolar growth is an issue. Implant placement prior to cessation of facial growth invites differential growth of the adjacent teeth, altering the original implant and crown position and thus affecting the eventual dental aesthetic treatment outcome. The orthodontist can measure cessation of growth with successive head films taken 6 months apart. Careful superimposition can determine cessation of facial growth.
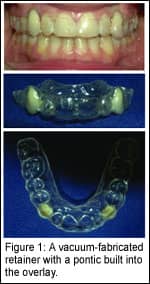
If facial growth, as seen in successive head films, is continuing, a “rock-solid” retention plan is critical. The classic retainer with an attached pontic invites selective tooth movement of adjacent teeth and can also be broken or lost.
In our pretreatment consultations, we advise the patient and parent that if there is a delay in implant placement of a few years, selective retreatment for a few months with additional braces may be needed to reposition the affected teeth. This is also applicable if the retention regime is not followed.
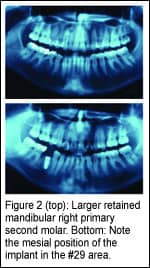
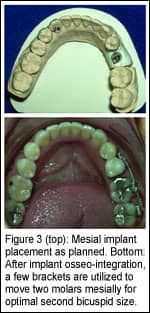
In some cases, there is more space opened prior to implant placement. This is typical in prosthetic replacement of a missing lower second bicuspid (Figure 2). When removed prior to implant placement, the larger, retained primary second molar will leave a mesiodistal space greater than the optimal size for the replaced smaller, lower second bicuspid. Work with your dentist and lab technician on implant location, anticipating the second bicuspid implant’s position in the edentulous area.
For an ideal-sized and ideal-placed second-bicuspid crown on the implant, residual space may need closure after crown placement. This can be achieved by adding a few brackets on adjacent teeth as well as the crowned implant, and by closing spaces. This often takes only a few months of additional orthodontic treatment.
Dental Implants Prior to Orthodontics
The Effect of Orthodontic Treatment on Gingival Tissue
The orthodontist must educate the referring dentist about dental aesthetic benefits of gingival symmetry. The
attractiveness of a smile comes not only from the color and shape of teeth, but also from gingival symmetry. In a healthy periodontium, the gingival margin of a tooth moves in concert with the tooth. This basic concept is an invaluable service to the patient, and allows for simple and effective alteration of asymmetric gingival tissue.
This is particularly evident in cases where the upper lateral incisor is missing and an upper cuspid is substituted into that site. Yes, there is often dental asymmetry (shape and color contrast
between the juxtaposed upper centralincisor and substituted cuspid), and also gingival asymmetry (the occlusal-gingival disharmony between those teeth as well as with the upper first bicuspid).
We educate our clients about this issue prior to orthodontic treatment. Our orthodontic outcome is to intrude the upper first bicuspids out of occlusion to move the CE junction more gingivally, simulating a true cuspid gingival margin and extruding the substituted cuspid, allowing its gingival margins to be placed more incisally to simulate a natural lateral incisor gingival contour (Figure 3).
After the gingival architecture is established, the infraerupted first bicuspids can be built up in composite and provide occlusion not only in centric relation, but also in providing anterior disclussion during functional jaw movements. This prosthetic work can be done in composite for the short term or with veneers for a longer-lasting outcome. The size and shape of the substituted cuspids and incisors dictate the type of restoration.
The concept of using dental intrusion to improve gingival margin symmetry prior to veneer fabrication is a tremendous orthodontic service to your restorative dentists and to their patients. The orthodontic treatment often takes less than 6 months, and adds considerable aesthetic value to the finished veneer work. This helps to meet the team’s dental aesthetic treatment goal.
This article is an attempt to share just a few principles and ideas with your team, based upon our defined treatment goals. As surgical techniques and dental materials continue to improve, all members of your team must be aware of changes in technology, so that all of your patients experience optimal dental care.
Straty Righellis, DDS, is an associate clinical professor in the orthodontic department at the University of the Pacific, and in the orthodontic division of the University of California at San Francisco. He is a past president of the Northern California Component of the EH Angle Society, and maintains a private practice in Oakland, Calif. He can be reached at [email protected].










