by Greg Thompson
Jimmy C. Boley, DDS, MS, speaks his mind about extraction, evidence, and practicing into his 70s
 |
For orthodontists who began treating patients during the Johnson administration, the technological changes within society and dentistry have been nothing less than revolutionary. Jimmy C. Boley, DDS, MS, who has been in private practice for the past 45 years, has seen his share of gadgets come and go. Through it all, he has refused to embrace any philosophy or technique that was not backed up by sound evidence.
While many advancements—lasers, 3D imaging, and new methods—have undoubtedly improved orthodontics, some fundamental truths about biology and the relationship of teeth to jaws remain unchanged. Boley contends that too many clinicians fall victim to trends, instead of recognizing these truths.
For example, if you routinely put in large flexible archwires for significant expansions of the upper and lower arch, Boley hopes you have first demanded compelling evidence that you are achieving the classic goals of orthodontics: good aesthetics and healthy, functional, and stable dentition. Ultimately, the decision to expand goes hand in hand with the ongoing extraction versus nonextraction controversy, a debate that refuses to go away.
The perspective of practicing in five separate decades reveals a pendulum that, much to Boley’s chagrin, often swings toward treatment preferences that have little to do with clinical documentation. The extraction controversy centers on the question of how best to gain space and resolve tooth-size-to-arch-length discrepancies (TSALD) and/or correct procumbent anterior teeth.
PRACTICE PROFILE
Name: Jimmy C. Boley, DDS, MS
Practice Name: J.C. Boley, DDS Inc
Location: Richardson, Tex
Specialty: Orthodontics
Patients per day: 45
Starts per year: 120
Years in private practice: 45
Days worked per week: 3
Office square footage: 2,800
Web site: boleyortho.com
Should orthodontists remove tooth structure or increase arch length? “I believe there are basic truths of nature that apply to most of our typical patients,” Boley says. “These laws should be considered when making the decision of whether to increase arch length. Much of these phenomena are so well documented that there should be little question in these areas.”
When questions do arise, Boley calmly explains his rationale in famously direct and no-nonsense presentations, such as the one he gave at the 2009 AAO Annual Session in Boston. During one recent talk, he outlined five questions to ask when addressing arch length and extraction:
- Do expanded mandibular canines tend to decrease in width post-retention?;
- Do advanced mandibular incisors tend to upright post-retention?;
- Does an expanded mandibular arch tend to return to its original form?;
- Does arch length typically decrease from mixed dentition to the permanent dentition?; and
- Does the mandibular arch tend to shrink throughout life?
If you answered yes to all five questions, you’ll get the professorial nod. If not, be prepared to present a convincing argument that relies on more than anecdotes. “These well-documented phenomena seem to support the theory that malocclusions are in equilibrium with their environment,” Boley wrote, “and we should strive to align and occlude the teeth with only minimal alteration of the original mandibular archform.”
Tradition and Texas
 |
| “I’m still pretty passionate about doing it [orthodontics] the traditionalist way,” Boley says. |
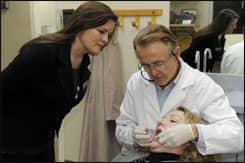
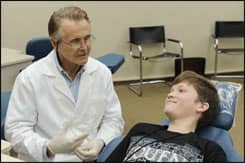
Based in Richardson, Tex, the 72-year-old Boley is a self-professed traditionalist who teaches in the orthodontic department at Baylor College of Dentistry in Dallas when he is not tending to patients at his 2,800-square-foot practice. He also frequently hits the road to spread his evidence-based gospel. Boley, a 2010 recipient of the Martin E. Dewey Award, is particularly well known for his strong views on the extraction question.
With little patience for clinicians who sacrifice quality of treatment on the altar of efficiency and convenience, Boley has no plans to stop saying what some orthodontists do not want to hear. “If teeth are more than slightly crowded and/or procumbent,” Boley says, “it is better to remove tooth mass than to increase the lower arch perimeter any significant amount.”
The problem is that studies show that the lower arch returns “fairly close” to its original form. “Another thing is the mandibular arch length is greater in the mixed dentition than it is in the permanent dentition,” Boley adds. “If you have a TSALD in the mixed dentition, and the arch length is going to be less in the adult dentition, does it make sense to temporarily increase arch length in the mixed dentition in order to align the teeth?” Boley asks. “Bob Little reported on this approach in the May 1990 AJO/DO, and found it produced the poorest long-term stability of any approach they studied.”
 |
 |
 |
For orthodontists who insist on expanding the lower cuspids, Boley says without hesitation that you can’t expect them to stay. Why bother when they will likely return to, or close to, the original position? The answer, he says, is ease of treatment, and that should never take precedence over results. “If you read people’s advertisements,” Boley says, “when they are trying to sell you appliances or approaches to treatment, they are usually touting earlier, easier, and with less work and effort.”
Boley has nothing against shortcuts. The problem is those supposedly time-saving techniques might get you lost. The final destination is what counts, and if that means taking the long way, patients will understand.
In borderline extraction cases—Boley’s signature issue—he says orthodontists nowadays want to squeeze teeth in rather than take them out. “I think the tendency is a little bit excessive on not taking out the teeth,” Boley explains. “I think we would be better off, especially in some of those borderline cases that are more crowded, to go in and take out the second bicuspids. The typical tooth that you take out in crowded or protrusive cases, where the teeth are sticking out, is the four first bicuspids. On those borderline cases, go ahead and take out the second bicuspids. That’s a compromise between not taking out any teeth and taking out the four first bicuspids.”
It all goes back to the pendulum that swings almost imperceptibly through the years. A few decades ago, clinicians may have erred on the side of too many extractions, whereas today it can be argued that the opposite is true. “The problem with taking out teeth when you don’t really need to is that you can end up with the teeth too far back in the mouth,” Boley says. “Nowadays, however, you see teeth sticking out too far where kids can’t close their lips over their teeth without mentalis strain.”
Great Results or Just Easier?
Does new technology make outcomes better, or simply smooth the road to the finish line? The distinction is a crucial element of Boley’s career-long dedication to patients. All that talk about low friction in appliances? Boley is not impressed, saying the supposed benefit amounts to little more than marketing hype.
According to Boley, even the paradigm-changing switch from bands to bonding, while certainly making things easier, did not appreciably change the quality of a patient’s smile. Ditto for flexible wires. “Some of the cases I treated 40 years ago are just as good or better than the ones I’ve treated now,” says Boley, who last year served as president of The Edward H. Angle Society of Orthodontists. “The technology that is going to make us get better results, and it is probably still in its infancy, are those miniscrews, also known as temporary anchorage devices (TADs). That is something really new and different.”
Despite his bracingly honest outcome-based philosophy, Boley acknowledges that for selected patients, new technology such as Invisalign® is effective and popular with patients. Lingual braces have also helped in the mission to attract adults. “The first lingual course I took was in 1983, so I’ve been doing it since then,” Boley says. “They have some new versions of the appliance out now that I think are a little easier. The lab bills are outrageous on the things. On a real hard case, it’s tough to get as good of results [with lingual], but on easier cases it is not a problem.”
 |
 |
Staying Chairside
While patients may be getting older, so too are orthodontists, who increasingly are choosing to stay chairside longer than ever. Boley is a part of the no-retirement trend, a phenomenon attributable to genuine passion for the profession. “I plan on selling the practice with the provision that I can work at least 1 day a week from now on, or as long as I still enjoy it,” Boley says with a chuckle. “I like the challenge of seeing if I can get those darn teeth straight, and I can do it fairly well. Yes, I’m still pretty passionate about doing it the traditionalist way, and with my lecturing and teaching, I figure if you are not doing it you don’t have much credibility.”
Building on that credibility during speaking engagements is a key to Boley’s continuing success during the four or five trips he makes every year. Receptivity to his message usually depends on the age of the listeners. Those middle age and older are all ears, but some “youngsters” can be a bit resistant.
Those who simply want procedures that are “quicker, easier, and faster” may not be as receptive. With cold logic and a Texas twang, however, Boley manages to earn their respect if not their full agreement. Swaying conference attendees is but one source of satisfaction. Ultimately, it comes down to seeing the results. “Having a real hard case turn out really well,” Boley says. “That is the thing I like most about orthodontics.”
Working with patients has always been fulfilling for Boley, but he admits that keeping staff members happy can be a dicey prospect for any practitioner. What’s the secret to harmony? “Underwork them and overpay them,” Boley says only half joking. “But seriously, the hardest part of orthodontics is keeping your staff happy. Fortunately, our people get along really well most of the time. Two of them started with me in 1969. Another started in 1982. I must be doing something right. Accept that they are not going to do everything precisely as you like, but if they do the majority of what you like, try to overlook the rest.”
If he ever actually sells the practice and only works 1 day a week, you may find Boley on the golf course a bit more often, where the 16 handicapper considers it a good day if he breaks 90. But if he still enjoys it, and is physically able, patients in the Dallas/Fort Worth metroplex will still be benefitting from Boley’s hard-earned wisdom for years to come. The 16 handicap may not come down, but the smiles he receives will be reward enough.
Greg Thompson is a contributing writer for Orthodontic Products. For more information, contact
 |
IN HIS OWN WORDS
In the following lecture excerpt, Jimmy C. Boley, DDS, MS, gives additional insight into the ongoing debate over when to extract and when to expand.
“I think a good solution to the extraction/nonextraction controversy is to extract all four second premolars in the borderline problems. These are the patients with good-to-slightly-full profiles and slight-to-moderate crowding of the mandibular incisors. Care must be taken with this approach so as not to retract the mandibular incisors more than you want. Frequently, managing a burn anchorage problem requires as much vigilance as a maximum anchorage problem. In these patients, normally it is desirable to maintain the mandibular incisors in their original position or not retract them over a couple of mm.
“The mechanics I use to handle this type of problem is to work up to maxillary and mandibular closing loop arches, and close both arches at once. If the mandibular incisors start going lingually too much or I am afraid they might, I close one arch at a time. The mandibular arch is closed first with enough Class II elastics to maintain the original overjet. If the overjet starts increasing, the patient needs to wear his elastics more. Once the lower arch is closed, the upper arch is closed, usually without any or much elastic wear.”