Cone-beam computed tomography (CBCT) has now been available in North America for more than a decade, and in that time it has become a vital part of many orthodontic practices, bringing added value to pretreatment diagnosis and treatment planning. The fact is CBCT provides a clearer view of patient anatomy and pathology, without the distortions or superimpositions of conventional imaging.
Orthodontic Products asked four orthodontists—Theodore Freeland, DDS; James Mah, DDS, MSc, MRCD, DMSc; David E. Paquette, DDS, MS, MSD; and Orhan C. Tuncay, DMD—their views on the use of CBCT and how it has impacted their clinical practice.
The oft-quoted remark from the newer as well as the older users of CBCT is, “I can never go back.” Why is that?
Freeland: I have been using LCBCT (limited CBCT) imaging for approximately 8 years. The ability to diagnose orthodontic cases is increased enormously. With one data set one can look for disease process and diagnosis the joint status. All the structures in the field of view can be measured in both 2D and 3D. The standard orthodontic images can be created in 2D.
The best part, however, is the generated images are actual size, so parts can be measured more accurately. The nerve canals can be located and mapped. Along with the use of 3D facial mapping technology, the entire head, both the soft and hard tissues, can be assessed. The volumetric size of the airway can be determined. The DICOM data set can be orientated to the natural head position for facial assessments. The pre- and post-DICOM data can be superimposed to assess the success of treatment. Never before has there been a technology that will allow the orthodontic profession to do so many things with just one tool.
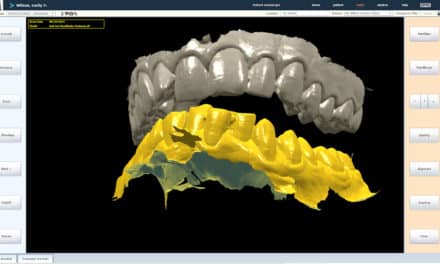
Mah: Since CBCT was introduced in North America in 2001, I’ve interacted with hundreds of CBCT users on the topic, and I have never met anyone that used CBCT and decided to go back to traditional dental imaging. Users generally describe 3D visualization as a remarkable experience where they can see patient anatomy clearly without the superimpositions, distortions, and magnifications associated with traditional imaging. This is often referred to as the “anatomic truth.”
Users generally feel that this technology is much more reliable and eliminates much of the guessing and assumptions associated with traditional imaging. This opinion is supported by the many studies reporting superior diagnostic specificity and sensitivity of CBCT relative to traditional imaging. Software tools allow for creation of traditional views as well as custom views for analysis of implant sites, dental impactions, sinuses, and temporomandibular joints. Add to this the abilities of relative bone density evaluations and the creation of models of the dentition, jaws, and face, and users have newfound capabilities for diagnosis and treatment.
Integration of high-quality laser scans of stone models and photographs in the model allow for a vast array of additional functions such as treatment simulations, communications, and manufacturing of surgical guides. As users gain experience with this technology, they tend to utilize it and its capabilities more and more and feel they make better treatment decisions. Given the above, it is not surprising that users of CBCT remark, “I can never go back.”
Paquette: I would agree. There are multiple reasons. The first and most useful thing is to know where the roots are in three planes of space when planning treatment mechanics. Secondarily is the benefit of identifying less common, albeit frequent findings, such as impacted canines, odontomas, or supernumaries, and of having a clear picture of what impact they may have on treatment.
Additionally, the ability to evaluate airways is becoming increasingly important. Finally, the ability to identify other rare abnormalities and make the appropriate referrals benefits patients.
Tuncay: Orthodontists are three-dimensional thinkers. In the earliest days of orthodontics and studies of craniofacial growth, they formed facial casts in an effort to view the patient in 3D near-life simulation. Then, in the early 20th century, Justus Antoni Wilhelm van Loon designed a way to orient dental casts behind the facial casts. It was laborious, but it is the great grandfather of much of our image-based recreations. In 1929, Holly Broadbent and Wingate Todd introduced the cephalometer to orthodontics, which was followed by photographs and, later, panoramic radiographs. All these were easy, especially, compared to working with plaster.
Inevitably, the orthodontist had to make the switch to visualize and reconstruct these two-dimensional images into a three-dimensional form in her/his own head. It became a habit to see the 2D images in 3D. It was a “qualitative” reconstruct.
This unspoken reconstruct stayed with the clinician despite a plethora of quantitative analyses of distances and angles on 2D images to study the patient and treatment results. Deep down, they knew it was not right to go by 2D measurements, but they didn’t yet have a better and easy system. And it helped to stay with the 2D images when it became difficult to justify multiple exposures to ionizing radiation.
Interestingly, despite all this, the orthodontist never lost the yearning for 3D images and information to diagnose and treatment plan better, let alone treat better.
It is tempting to posit orthodontists never lost this desire because they are human beings with a stereoscopic vision. It is a primal urge to see the world in 3D. Reconstructs from 2D images in the brain cortex, at best, are a substitute. Thus, this primal urge to see the objects in 3D is the primary reason orthodontists say they can’t go back.
What sort of education do you provide to your patients before taking CBCT images? Also, do you use a consent form?
Freeland: It is explained to the patient that the use of CBCT is similar to having a panoramic radiograph taken. The total event is explained. Moreover, the patient is educated on exactly what is going to happen during the image-acquisition stage. The only drawback to acquiring an image is they have to hold absolutely still. So a considerable amount of time is spent on explaining how long it will take and what the machine will be doing. A consent form is used that covers all the records that are taken for their diagnosis.
Mah: We describe the technology to patients and explain to them that it provides us with comprehensive information relating to their jaws, joints, air spaces, and teeth, and allows us to diagnose and plan in more detail. We have never had a patient refuse the imaging. Indeed, at the University of Nevada, Las Vegas, we have surveyed patient opinions relating to the level of education provided to them regarding CBCT imaging, and they responded very positively. In addition, they felt more highly of the clinicians providing CBCT and his/her abilities.
We have a consent form for treatment that includes radiographic imaging. We do not believe a separate consent is warranted for CBCT imaging. Radiation dosimetry studies show that the effective absorbed dose is in the same range as a traditional dental imaging series and is much less than full-mouth examination.
Paquette: I do not use a consent form and provide the same information I would prior to taking any other image.
Tuncay: Patient education happens at the initial visit, in the form of showing the patient 3D images from a scanner, as well as the CBCT. We then point out and explain how certain conditions could not be diagnosed in the 2D images and how it is beneficial to know those. The patient subsequently becomes a committed spokesperson for the excellence of the practice, especially if the radiologist reports unusual calcifications, bone problems, unusual formations, or growths. Patients can tell their physician their condition was actually discovered by their orthodontist.
The ortho-dentist aligns the crowns of teeth in the mouth; the visible part. In contrast, the job of the orthodontist is to align the roots. To explain this fact to the patient with the aid of images is invaluable. Just as the orthodontist wants to see in 3D, so does the patient.
Reading of 3D images by a radiologist is often recommended. How have these reports affected your practice? Have you ever received reports of conditions that you had totally missed? Can you comment on any interesting experiences?
Freeland: The use of a secondary interpretation is a must. A two-level system is employed. When starting CBCT, I took courses in how to read and use the data. The courses included sections on pathology. If I see something I think is suspicious on the axial, coronal, or sagittal data, I send the DICOM file by Internet to BeamReaders. The reports have helped with diagnosis and treatment decisions. So far, I have not missed anything I know of.
The most interesting area is the temporomandibular joint. It was a total surprise how many patients between the ages of 8 and 14 have some signs of condylar change. Some cases are active regressive joint disease, and others show a change in shape from a malocclusion.
Mah: Establishing a working relationship with an oral maxillofacial radiologist (OMFR) is definitely recommended. Most clinicians work with an “interdisciplinary team,” and an OMFR should be included. Radiology reports serve not only as a record that the entire volume was interpreted but also helps to reduce the tendency toward “tunnel vision” toward the specific region of interest and ignoring other regions of the volume. At the university, I have many examples of missed findings.
For example, an implant imaging series that completely missed a tumor in the esophagus, an orthodontic evaluation that missed a dentigerous cyst, and a TMJ series that missed calcifications in the carotid plexus. Indeed, our 2007 study of over 500 consecutive patients showed that in full-field-of-view CBCT scans, incidental pathology was found by an OMFR 25% of the time. Even for experienced users, the OMFR serves as a second set of eyes viewing the data.
The two areas where radiology reports have helped the most are for variations of normal anatomy and pathology. In the former, CBCT serves to illustrate that there is great anatomic diversity among patients, and the reports help to confirm if the finding is a range of normal or not. In the latter, the OMFR is also invaluable to assist in establishing a differential diagnosis and an appropriate course of management.
As far as interesting findings, there are many, many experiences that I can think of. These vary from variations of anatomy such as minimal alveolar bone supporting the teeth to the point of perforation between the buccal and lingual cortical plates; impacted teeth in the ethmoid sinus, palate, coronoid process, and the condyle; foreign objects such as vascular clamps, bullet fragments; and various craniofacial anomalies and pathologies.
Paquette: I initially used radiologists very frequently. After years of reviewing CBCT images, I have learned that much of what I was unfamiliar with was simply a more accurate image of some variant of normal anatomy. I have not received any reports that have revealed any conditions that I have missed. However, they have diagnosed conditions where I recognized something on the image that was abnormal. Although CBCT images have changed multiple treatment plans during any given month, a radiologist report has not affected my practice.
Tuncay: I preach and practice that all CBCT images are sent to a radiologist. Exceptions may be limited field-of-view exposures such as single-tooth exposures, TMJ images, and the like. The orthodontist is sufficiently trained in the dental school to read those.
Interesting and missed experiences are common. Just about every orthodontist who uses CBCT would have stories to tell. My stories fall into the category of “ordinary.”
Several published papers offer cephalometric analyses of some sort, and most of them employ linear dimensions for measurements. What do you make of using these tools of planar geometry in a 3D image? Do you have any use for them?
Freeland: A CBCT cephalogram created from DICOM data is much more accurate. If the image were created using the orthogonal view, all measurements are one-to-one. There is no magnification such as a regular cephalogram. Incorporated in the software are measuring tools that can be used on the 3D model. One example is determining the size of the maxilla transversely compared to the mandible for deciding if palatal expansion is needed. Another area is locating asymmetries.
For example, cases that present with one side Class I and the other side is full-cusp Class II with a midline shift to that side. The mandible can be measured to help determine if the problem is from an odd-shaped mandible, or if the problem is the result of a cranial base asymmetry. The use of linear measurements can be applied to anterior/posterior vertical dysplasia to determine the extent of a fulcrum.
Mah: The linear dimensions developed with traditional cephalometry generally remain valid when they are employed with CBCT data. The forefathers of cephalometrics knew that image magnification was a significant error and made efforts in cephalostat design to reduce this. The x-ray source was positioned at a distance from the patient in an effort to generate more parallel x-ray beams and to reduce magnification between left and right sides.
In addition, cephalometric analyses utilize many angles that are not affected by magnification. Linear measurements are affected, and for this reason, many of them are very short distances in the order of a few millimeters, so the 5% to 9% magnification associated with cephalometrics is not significant. This leaves the longer linear measurements that may be affected, such as Harvold’s mandibular length or sella-nasion. Therefore, one must use these with caution, albeit, long linear measurements in cephalometrics also generally have very large standard deviations.
Until population databases of CBCT data are developed, the conventional cephalometric analyses will continued to be utilized. Researchers are investigating both qualitative and quantitative three-dimensional analyses of CBCT data to establish new methods of assessment.
Paquette: I think the analyses may be helpful for a research project, but I have little use for them in day-to-day practice.
Tuncay: Here is a message we must get out to the orthodontic community:
- 3D images deal with surfaces.
- More important to understand shape and surface topography.
- 3D images provide a bounty of qualitative information.
- Measurements of distances and angles are the tools of planar geometry, not of solid geometry.
- In 3D, we are in a world of voxels; not pixels.
- 3D images are better studied with finite volume analyses (FVA); not finite element analyses (FEA).
- Methods of (functional) animation of 3D images need to be developed. OP