by Alfredo Gilbert, DDS, MS
A lingual treatment protocol in 10 steps
 |
Lingual orthodontic cases represent a challenge from both the aesthetic and functional points of view. Those of us dedicated to resolving malocclusions with this technique understand just how delicate the movements can be, and how serious the consequences of these movements can be for the evolution of the cases. Extreme caution is required in each and every step in order to achieve the desired result. Errors can be costly due to the resulting prolongation of the treatment time and associated difficulties.
The treatment protocol described here extends from patient selection to the conclusion of the case. It includes a novel finalization procedure that I designed, which ensures greater control during the finishing stage and thus a more reliable and standardized level of excellence.
 |
| Alfredo Gilbert, DDS, MS |
1) Elaboration of the Clinical History and the Treatment Plan
During the elaboration of the clinical history it is essential to pay special attention to the relevant psychological aspects in order to determine whether the patient suffers from bruxism or tongue habits. Bruxism is a clear indicator that the patient vents his or her neurosis through the masticatory muscles.1 Any tongue habits that tend to open the bite may need to be controlled by the use of a crib (Figure 1).
Once I have established the clinical history, carried out the diagnosis, and designed the treatment plan, I take a facebow record in order to mount the case in a semiadjustable articulator. Every clinical case must include mounting the cast in the articulator.2 The obstacle that lingual brackets represent to the dental occlusion may mislead the operator and perturb the patient, and thus a skeletal record is preferable to exclusively dental records. Carrying out a cephalometric conversion in the relevant cases leads to more precise information about the malocclusion.3
 |
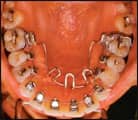 |
| Figure 1: Any tongue habits that tend to open the bite may need to be controlled by the use of a crib. | |
The treatment plan in lingual orthodontics must consider topics that are not commonly analyzed in labial treatments. One such topic is the concordance between centric relation and centric occlusion, a topic whose importance may be appreciated when we note that most lingual orthodontic patients are adults, and that a great proportion of adults, whether through loss of teeth or altered teeth morphology due to wearing or reconstructions, present a discrepancy between the skeletal and dental records.
The fact that the lingual apparatus impedes the anterior settling of the teeth poses a problem that manifests as loss of vertical anchorage, loss of anchorage of the canine guide, and loss of the ability to use the temporomandibular joint as a reference point. It is thus imperative to take the face-bow record before mounting the cast in a semiadjustable articulator (Figure 2).
 |
 |
| Figure 2: It is imperative to take the facebow record before mounting the cast in the semiadjustable articulator. | |
2) Decreasing the Load-Deflection Rate
Before sectioning the models, I elaborate the round archwires over the patient’s original malocclusion. This helps avoid the problems caused by a poorly fitting archwire. Four mechanisms are used to decrease the load-deflection relation of an archwire4:
- Increasing the interbracket distance is achieved using brackets with reduced mesiodistal dimensions. Being able to introduce brackets into all of the slots allows rotations to be corrected more quickly; however, control during retraction is usually compromised, above all when the spaces are large.
 |
| Figure 3: Using shape-memory alloys. |
- Reducing the caliber of the wire also facilitates inclusion in most of the slots. Round wires do not enable control of torque, and their use is therefore limited to the correction of rotations.
- Increasing the length of the wire via the multiloop technique is somewhat troublesome in lingual orthodontics. Insertion of the wire is extremely difficult, and the irregular wire is uncomfortable for the patient.
- Using shape-memory alloys allow orthodontic treatments to be completed in shorter times and with fewer troubles for the patient. Annealing a Nitinol wire at a temperature of 600°C (1,112°F) facilitates bending without causing the wire to lose its capacity to undergo the reversible martensitic/austenitic transformation characteristic of such alloys (Figure 3).
3) The Setup
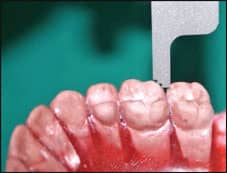 |
| Figure 4: The setup should be elaborated according to the norms stipulated in phase III of the ABO examination process. |
When you consider that brackets are usually prescribed through the use of a setup, and that lingual orthodontic treatments are realized “retrospectively,” then it is logical to create the prescription in the most exact manner possible. With this in mind, the setup should be created according to the norms stipulated in phase III of the ABO’s examination process—that is, it should be treated as a case-finalization project (Figure 4).5
The positions of the setup can be verified using a Ray Set goniometer. This appliance permits calculation of the angles at which the teeth are positioned in the model. I use the Ray Set after elaborating the setup to verify that the positions are in accordance with the treatment plan. I designed a removable tray so that the models can be easily transferred between the Ray Set and the articulator (Figure 5).6
4) Biomechanical Considerations
 |
| Figure 5: The Ray Set verifies that the positions are in accordance with the treatment plan. |
The occlusal interference caused by the brackets, the irregular form of the archwire, and the variations in the distance between the point of application of the force and the tooth’s center of resistance (usually shorter in the lingual case) mean that the biomechanics of lingual orthodontics are much more complicated than those of labial orthodontics. The appliances to be used and their bonding positions must be selected on an individual basis, taking into account the patient’s dentoskeletal characteristics, malocclusion classification, and facial morphology.7
The two factors that especially complicate lingual biomechanics are 1) the shorter distance between the point of force application and the center of resistance of the tooth; and 2) the internal insertion of the wire. Pushing instead of pulling provokes loss of control of the movements.
Consider as an example the case of a patient possessing an alveolar bone of lower than average height. The moments of torque and rotation will be altered by the modified distance between the position of the bracket and the center of rotation. In such cases, using round wires tends to increase the overjet and to open spaces. Rectangular wires should be inserted as soon as possible to promote bodily movements with greater control.
On the other hand, patients requiring retraction need appliances that permit opening of the bite to prevent contacts in the occlusion. However, it is probable that these same appliances represent an interference that impedes closing of the bite during the finalization stage, and thus necessitate some sort of compensatory adjustment, always respecting the difficulties inherent in mobilization “from within.”
 |
| Figure 6: The brackets of Class II, Division 1 patients should be bonded in the positions indicated by the ideal arch. |
The brackets of Class I patients whose anterior teeth present correct inclination are bonded in such a way as to not disrupt the dental occlusion. On occasion, we raise the bite with glass ionomer. This means that frequently the appliances are located gingivally to the ideal point determined by Andrews8 for the straight-wire technique, with the consequent risk of altering the force moments and couples by decreasing the distance to the center of rotation. Sometimes the shorter distance to the center of rotation may be increased by adding thick resin bases that allow standardization of the buccolingual diameters of the anterior teeth. By locating the center of rotation in the panoramic radiograph and measuring the thickness of the resin bases, you can calculate the moments to generate and, if necessary, adjust the positions in the setup.
5) Class II, Division 1 Patients
The brackets of Class, II Division 1 patients should be bonded in the positions indicated by the ideal arch. I use the semiadjustable articulator to verify that there will be no contact with the bite planes of the anterosuperior brackets. Contact here could occasion a greater proclination of the anterosuperior teeth. When the brackets are bonded, I advise the patient that the appliances should represent a buffer for the inferior incisors, and that the mandible should not be pushed forward excessively. For those patients presenting an open bite, I recommend the use of a tongue crib.
The archwire design requires bends next to the distal ends of the tubes to prevent proclination of the anterior teeth. In cases of premolar extraction, the compensation between the canine and premolar should be slightly distalized to permit retraction. Patients with multiple absences require a personalized wire design (Figure 6).
 |
 |
| Figure 7: The brackets of Class III patients are bonded as close as possible to the positions indicated by the ideal arch. |
6) Class III and Class II, Division 2 Patients
The brackets of Class III and Class II, Division 2 patients should also be bonded as close as possible to the positions indicated by the ideal arch.
Class II, Division 2 cases present an inherent biomechanical complication. The point of force application is “forward” of the center of rotation, so that the force moments tend to lead to greater reclination of the dental crown. This problem can be resolved by the bite planes of the brackets, which in this case act as inclined planes, projecting the anterosuperior teeth forward. The choice of apparatus is crucial here, since brackets that do not adequately raise the anterior teeth will complicate correction of the reclination (Figure 7).9
7) Bracket Positioning
I recommend the bracket-positioning system designed by Hiro. I have found it advisable to make the modifications to the systems described above as well as those necessary to elaborate the individual guides.
The morphological irregularity of the lingual surfaces makes the use of indirect bonding systems inevitable.10 Only this method possesses the precision needed to standardize the buccolingual widths. I prefer to use standard brackets, to which information may be given in order to convert them to pretorqued and preangled brackets, thus realizing the individualized prescription determined by the treatment plan.11
8) Monitoring
Monitoring lingual cases is similar to monitoring labial cases. Every 4 to 6 months, casts, photographs, and radiographs should be taken to monitor changes in angulations and torque. If I find anything too different from what I expected, I try to recover the position as soon as possible. It has been noted that the bite planes of the anterosuperior brackets usually function as an occlusal buffer, preventing the patient from leaving centric relation.
I constantly check for the symptoms of joint lesions: the appearance of pain, crepitating, or sounds in the temporomandibular joint. Upon discovery of one or more of these symptoms, I proceed as appropriate, on occasions prescribing some type of anti-inflammatory or even suspending orthodontic treatment and using acetate with acrylic, which functions as a myorelaxant.12
 |
 |
||
 |
 |
||
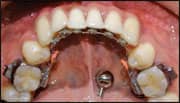
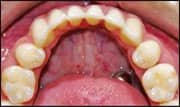
| Figure 8: Entering the final stage of treatment, which involves detailing the case and coordinating the arches. | |||
9) Finalization
Lingual orthodontic treatments may be divided into two stages: a rough stage and a refining (or detailing) stage. The rough stage consists of aligning, leveling, retraction, bite opening, and correcting rotations and the occlusion. The refining stage consists of achieving root parallelization and the best occlusion possible.
In labial orthodontics, the objectives of the refining stage are achieved with the aid of a panoramic Rx from which the root parallelisms may be evaluated. Lingual orthodontics requires a much more extensive procedure. The presence of brackets on the palatine surface of the anterosuperior teeth makes it difficult to evaluate both the anterior settling and the dental articulation.
When I arrive at the detailing stage, I remove the caps of the brackets, take impressions with polyvinyl siloxane, take face-bow records, and mount the casts in the articulator. With these records and the information obtained from a panoramic radiograph, I can remove the brackets from those teeth with incorrect angulations.
I then carry out a new removable setup in which only the teeth with imperfections are cut and repositioned with wax. I use a new 0.018 x 0.025 archwire with the mold to fabricate the guides of those brackets to be repositioned. I rebond the brackets and fit a 0.016 NiTi wire fabricated in Memory Maker. With the space available owing to the absence of the bracket caps, I can detail the case and coordinate the arches (Figure 8).13
 |
| Figure 9: Retention must be considered as an active part of the treatment. |
10) Retention
Retention must be considered as an active part of the treatment. The control exercised during retention is essential to limiting changes to the finalization positions.
Given that lingual orthodontic patients do not accept visible retention appliances, I recommend using vacuum-formed thermoplastic retainers. These retainers have been demonstrated to adequately prevent relapse, a common problem especially in the mandibular arch. I do not, however, recommend using such retainers if the patient tends to bruxism. Fixed retainers should be used in those cases, bonded from canine to canine in cases without extractions, and from second premolar to second premolar if there have been extractions.
I teach the patient how to check the condition of the retainer at home, and then see him or her every 6 months in the clinic to carry out a thorough inspection (Figure 9).
Lingual orthodontics is constantly under the scrutiny of both the orthodontic community and the patients themselves. We must demand the highest standards of excellence in order to maintain the lingual technique as a viable treatment alternative. By following the protocol described above and achieving the objectives it sets out, your treatments will reach a more reliable and standardized level of excellence.
Alfredo Gilbert, DDS, MS, is a guest professor of lingual orthodontics at the Hospital Infantil du Mexico Federico Gomez and the academic coordinator of lingual orthodontics at the Facultad de Estudios Superiores at the Zaragoza campus of the Universidad Nacional AutÓnoma de MÉxico. His book, Lingual Orthodontics: The Truly Invisible Orthodontics, is available at amazon.com. He can be reached at
References
- Arnette GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning, Part 1. Am J Ortod Dentofacial Orthop. 1993;103:299.
- Stuart CE. Geometrics of the gnathic system. J Gnathol. 1982;1(1):6-8.
- Gregoret J et al. Orthodontics and orthognatic surgery: Diagnosis and treatment planning. Chapter 6: Cephalometric Conversion. Barcelona:Espaxs;113-120.
- Nanda R. Biomechanics in Clinical Orthodontics: Biomechanical Principles. Philadelphia: W. B. Saunders Co; 1997:1-21.
- Casko JS, Vaden JL, Kokich G, et al. Objective grading system for dental casts and panoramic radiographs. Am J Orthod Dentofacial Orthop. 1998;114: 589–599.
- Gilbert RA. A gonniometrical apply to review the setup of dental casts. Revista ADM. 2008;44(1):20-35.
- Scuzzo G, Takemoto K. Invisible Orthodontics: Biomechanics and comparative biomechanics. Chicago: Quintessence Books; 2003.
- Andrews LF. Straight wire: The Concept and the Appliance. Los Angeles: Wells Co; 1989.
- Gilbert RA. Lingual Orthodontics: The Truly Invisible Orthodontics. Mexico: Trillas; 2008:65–81.
- Aguirre, MJ. Indirect bonding for lingual cases. J Clin Orthod. 1984;18:565-569.
- Mestriner MA, Enoki C, Mucha JN. Normal torque of the bucal surface of mandibular teeth and its relationship with bracket positioning: a study in normal occlusion. Brazilian Dent J. 2006:17(2).
- Rubiano MC. Treatment with gnathological guards and occlusal corrections with selective reducing of the guard material. Venezuela:Amolca.
- Gilbert RA. Finalization in lingual orthodontics. Paper presented at: Annual Meeting of the American Lingual Orthodontics Association. May 16, 2008; Denver.
- Reitan K. Principles of retention and avoidance of post treatment relapse. Am J Orthod. 1969:55:776-790.
- Cerny R. Permanent fixed lingual retention. J Clin Orthod. 2001:35(12):728-732.










