By Jack C. Fisher, DMD, and Jay Burton, DMD, MBA

is better able to exert a force near the center of resistance of the alveolar processes of the maxillary bone, resulting in more horizontal separation of the mid-palatal suture and less dental tipping.
The Case for TSADs
The advent of rapid maxillary expansion (RME) as developed by Andrew J. Haas, DDS, allowed clinicians the ability to resolve posterior crossbites and improve archform by separating the mid-palatal suture.?Haas’s appliance not only had a? mid-sagittal jackscrew, which provided the force to separate the maxilla, but it also incorporated acrylic that is in contact with the keratinized gingiva of the palate. The purpose of the acrylic is to not only provide a force to the crowns of the teeth, but also to distribute that force along the alveolus and palatal vault nearer the center of resistance of the maxilla. This was in an effort to maximize horizontal separation of the maxilla, thereby limiting the tipping of the alveolus and teeth during the expansion phase.
A complication of this design is that tissue necrosis often occurs due to the pressure of the acrylic portion of the appliance on the tissue. Because of this potential complication, many? clinicians have migrated away from using the Haas appliance to a Hyrax-type appliance. The Hyrax appliance only exerts a force on the crowns of the teeth. This can result in more buccal tipping not only of the teeth but also of the alveolar processes. This type of expansion can thus lead to a less stable situation (ie, more relapse) and potentially contribute to the development of an open bite.
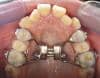
The placement location and direction of force dictate the appliance design to a large degree. In patients with unerupted or? partially erupted canines, the ?premaxilla is the area of ?choice for the placement of ?temporary skeletal anchorage devices (TSADs). Placement in this location allows the direction of the force to be approximately perpendicular to the long axis of the TSAD. In addition, a cap is not needed in the appliance design because of the perpendicular nature of force (figures 1a and 1b).


A third option is to place four TSADs—two in the premaxilla and two in the posterior maxillary alveolus, as seen in figures 4a and 4b. This would be the appliance of choice for a patient in the late teens due to the increase in force necessary to separate the mid-palatal suture.

If unilateral expansion is desired, the use of skeletal anchorage can be beneficial (see figures 5a and 5b). The TSADs are placed in the alveolus on the side where expansion is not needed. Bands are placed on the side where expansion is desired. When force is applied, more expansion will take place on the side with the bands than the side with the TSADs.

TSAD Expansion Appliance Clinical Protocol
Once the decision to use TSADs is made, the following protocol should be observed:
Visit 1: Separators are placed.
Visit 2: Fit bands. After bands have been fitted, an impression is taken and bands are removed and positioned in the impression to be poured in plaster. Once set, the exact placement location is marked with a pencil on the stone model and a small-diameter hole is drilled into the model exactly where the TSADs are to be placed. A larger hole is then bored approximating the depth of the soft tissue in the area of placement. This allows the base of the TSAD to be placed in the cortical bone, thereby increasing stability. TSADs that have been removed from a prior patient and sterilized are then inserted into the drilled holes in the model. This model is then sent to the lab for the construction of the appliance.
Note: Prior to TSAD placement, the clinician should do their due diligence in the selection of location for the TSAD. When planning the placement of TSADs, the use of ?limited-field-of-view CBCT DICOM images is the radiograph of choice. DICOM ?images allow the clinician to visualize the ?roots in all three planes of space and all other anatomical structures prior to placement, including cortical bone thickness, keratinized tissue thickness, sinus location and morphology, etc. However, a panoramic radiograph can be used if CBCT is not readily available.
Visit 3: Separators are placed.
Visit 4: One to 2 weeks after separators have been placed, the appliance is tried in before administering local anesthesia. When it is determined the appliance fits, anesthesia is administered. Do not remove the appliance. It remains in place and becomes a template for drilling the pilot holes. After the pilot holes have been drilled, the appliance is removed and a tissue punch is done to remove the keratized tissue in the area of placement. At this point, the TSADs are placed. The appliance can now be tried in for a second time to assure proper alignment of the appliance with the TSADs. Minor adjustments of the appliance loops are often needed with premaxillary TSADs. After this adjustment is completed, the appliance can be cemented and expansion can begin.
The patient and/or parent should be instructed to turn the appliance twice in the morning and twice in the evening. The patient will return to the clinic weekly until the desired amount of expansion is acquired.
After the desired expansion has been completed, composite is used to cement the jackscrew to prevent postexpansion relapse. At this point, the appliance remains in place for 6 months prior to removal.
Benefits of TSAD Expansion
Incorporating TSADs in RME appliances offers several advantages over the traditional Haas and Hyrax appliance. It is more hygienic than utilizing the Hass appliance because there is no acrylic incorporated into the design. The use of TSADs also allows the expansion to take place in a more horizontal direction since the force is directed closer to the center of resistance of the maxilla. This helps minimize the tipping of the teeth and/or the bending effect of the alveolus that often happens with the Hyrax type of appliance. A third benefit is the increase in the nasal volume and therefore the potential increase in the amount of air flowing through the nasal cavity.
Conclusions and Thoughts
These types of appliances should be utilized by clinicians with considerable experience with TSADs. The TSADs must not only be placed in the proper location, but must also be placed with proper protocol. The type and design of these devices when used for expansion anchorage is also important.
The specialty of orthodontics has undergone considerable change in the last 10 years. It is our opinion that skeletal devices—like the ones illustrated in this article—should be placed by the orthodontist. And this means that as the specialty continues to change, the training of the clinicians entering the specialty must also change. Orthodontic education must keep pace with the advancements that are being made. It is therefore the role of the orthodontist with this type of experience to make themselves available to program directors so that future residents may get the experience needed to grow with the specialty. OP
 |
Jack C. Fisher, DMD, has maintained a private practice since 1982. He can be reached at [email protected]. Jay Burton, DMD, MBA, is an orthodontic resident at New York University. He can be reached at [email protected]. |