by Michael J. Gunson, DDS, MD; G. William Arnett, DDS, FACD; and Dipak Chudasama, BDS, MSC, MORTH RCS, MBA
Developing clinical criteria to objectively judge aesthetic outcomes
 |
 |
 |
| Michael J. Gunson, DDS, MD | G. William Arnett, DDS, FACD | Dipak Chudasama, BDS, MSC, MORTH RCS, MBA |
Historically, science has tried to define the aesthetic face in its own terms. By quantifying beauty, science and medicine have attempted to treat aesthetic shortfalls with some repeatability and reliability. The problem with many of these past beauty analyses approaches has been either subjective bias or oversight of influential factors.
In the early years of orthodontics and orthognathic surgery, plaster models were the treatment-planning modality of choice. It was assumed that bite correction based on model diagnosis would achieve all facial and dental goals, including facial harmony. Experience has revealed that model diagnosis is incomplete.1-3 Model examination reveals interjaw occlusal discrepancies but does not indicate which jaw is abnormally placed. Because of this, model-based overjet correction may leave facial imbalances uncorrected or even create facial decline.1-3
As the model approach proved ineffective, a second diagnostic technique emerged. Numerous osseous cephalometric analyses were developed to diagnose and select correct treatment. The assumption here was that, by placing the skeletal parts within the range of skeletal cephalometric norms, facial balance would be achieved and the result would be beauty. Diagnosis of beauty by conventional osseous cephalometric norms is unreliable, however.3-5 These cephalometric analyses concentrate mainly on the measurement of hard-tissue structures that are not consistently related to the soft tissues of the face. In addition, when different cephalometric analyses are used for the same patient, conflicting diagnoses emerge. Each analysis provides a different diagnosis, a different treatment plan, and a different facial outcome. Treatment based on cephalometric hard-tissue norms in many instances may create undesirable facial changes.1-13
More recently, a third method of diagnosis has emerged. Clinicians have begun to select treatment based on direct facial examination and diagnosis.3,6 The assumption with this approach is that treating a face to “what looks beautiful” will produce a beautiful facial result. Models are analyzed and the hard tissues are evaluated, but the overriding key to treatment with this methodology lies in the clinician’s perception of the size, shape, and position of facial soft-tissue parts. While this kind of treatment-planning focuses attention onto where aesthetic problems truly exist, it is unfortunately rather subjective. Previously discussed analyses attempted to quantify beauty, with mostly unsuccessful results. Facially focused treatment-planning offers improved results but moves away from quantification. This allows subjective error to bias treatment-planning and outcomes. The aim of this article, then, is to discuss the elements of beauty and how each element influences the clinician’s perception of the face. By recognizing these influences, the clinician can overcome subjective bias and maximize the reliability and repeatability of beautiful results.
Quality and Position
Two factors influence the perception of beauty: the quality of facial parts (such as hair or eyes), and the position of the facial parts (including chin projection and symmetry).
The quality of facial parts makes the most significant impact on the perception of beauty. Quality is described with terms such as color, sheen, texture, and wave. The quality of the hair, eyes, eyelashes, teeth, gingiva, skin, and lips is of primary importance to beauty. Quality of parts is subjectively interpreted and can have a very emotional influence on the observer’s discernment of the face as beautiful or not. Alteration of quality is the thrust of most readily available cosmetics and procedures. Skin resurfacing, tooth bleaching, makeup, and colored contact lenses all modify the quality of facial parts. When quality is a dominant characteristic, whether positive (beautiful hair) or negative (facial acne), it will overwhelm the entire perception of the face and draw the viewer’s eye to it. For example, if a person has beautiful hair, his or her mildly recessive chin often goes unnoticed.
Position of parts is the next element of beauty. The spatial interrelationship of facial parts, including the forehead, orbital rims, cheekbones, subpupil cheek, nose, nasal base, lips, chin, and throat length, combine to create facial balance or harmony. Unless grossly out of balance (such as with severe chin retrusion), the spatial relationship of parts does not dominate the perception of beauty. Parts balance is subjectively and generally unemotionally interpreted.
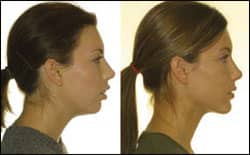 |
| Figure 1: Presurgical on left, post MSLFI and BSSO on right. On the left, the viewer’s eye is immediately drawn to the dominant negative traits (excess incisor exposure, large interlabial gap, and chin recession). On the right, the eye-catching quality is revealed once the dominant negative characteristics have been removed. The patient possesses beautiful quality (eye shape, color, skin tones) that is unmasked by the surgical correction of her dominant negative traits. |
 |
| Figure 2: Presurgical on left, postsurgical on right. Note the distracting dominant negative traits on the left. Postsurgery, the dominant negative characteristics have been corrected. The assessment of the postsurgical result is a combination of position of parts and quality of parts. |
Altering the position of facial parts involves more invasive procedures than improving quality. These include dental implants, orthodontics, rhinoplasty, and orthognathic surgery. As with facial quality, if the position of the part is a dominant characteristic, it will eclipse the other positive elements of the face. An example of this would be a severely deviated mandible: No matter the quality or position of the other parts, the eye is drawn to the chin deviation and the remaining elements lose their influence on the overall perception of beauty.
The interplay of quality and position of parts greatly influences the clinician. As mentioned, when the face is unconsciously judged, the dominant feature (quality more so than position of parts) draws immediate and distracting attention. This might be a positive trait such as beautiful eyes or a negative one such as extreme chin recession. Often, outstanding quality leads to the perception of beauty even when facial balance is marginal. The clinician will unconsciously forgive mild chin retrusion or nasal base weakness if the patient possesses full lips, smooth skin, or brilliant eye color and form. However, facial imbalance, when severe, such as severe chin retrusion, distracts attention from positive facial quality. The gorgeous eyes go unnoticed because the chin recession dominates the viewer’s attention. In general, the quality of facial parts automatically draws the attention of the clinician and is more important to the perception of beauty than the minor imbalance of facial parts’ position.
The clinician benefits from the dominant effect of facial quality. A patient who has severe position problems with unrecognized outstanding facial quality will have a more dramatic result. With the correction of the distracting imbalance of the parts, the quality of the patient’s face is unmasked, and the surgeon’s final result appears more remarkable. Many times, after treatment, patients and those who are close to them notice for the first time just how vibrant the patient’s eyes really are.
On the other hand, quality can adversely influence the treating doctor’s perception of the adequacy of the treatment results for many of the same reasons. The influence of quality on the clinician’s eye can distract from minor position-of-parts problems and leave them untreated or unrecognized after final treatment has been achieved.
And finally, if poor quality existed prior to surgery and its improvement was not part of the overall treatment plan, the clinician’s efforts will not be as satisfying as they otherwise could be. Perfect facial balance will not appear as “beautiful” unless attractive facial quality is present. Quality of parts is what gives the emotional component necessary for extreme beauty.
Measuring the Face
Without some means of either masking quality or quantifying the exact position of parts, error and bias will influence the clinician at all levels of treatment. Unfortunately, contemporary surgery and orthodontics often do not produce optimal facial balance, because facial part changes are subjectively planned and assessed rather than objectively measured. Without objective presurgical and postsurgical measurement of the interrelationship of facial parts, there will be a failure to recognize optimum facial balance.
The face is not measured for multiple reasons. First, an accurate method of measuring the position of facial parts is not in widespread use. Also, clinical soft-tissue measurement is difficult. And finally, overjet correction rather than soft-tissue balance remains the standard for most treatment planning.
In the past, a few soft-tissue cephalometric analyses have been developed to measure facial positions.7-10 These early soft-tissue analyses were not combined with clinical assessment, nor did any one of them examine all of the important facial components. Recently, facial balance and beauty diagnosis and planning have been improved by means of a combination of clinical facial analysis3,6,12 and soft-tissue cephalometrics11-12 (STC). STC ensures objectivity by directly measuring the relative position of all the facial parts involved in treatment. It also provides normal values, emphasizes soft-tissue outcome, removes the subjective influence of preexisting quality, and lessens the emphasis of overjet as the sole indication of success. Using STC focuses the diagnosis and the result on what orthodontics and surgery can change: the interrelationship or balance of parts. Beautiful quality such as skin, hair, or lips cannot obscure poor orthodontic or surgical positioning of facial parts.
Facial beauty is a combination of quality, position, and balance of parts. A variety of faces and profiles are aesthetic if the right combination exists. It has been stated in the literature that attempting to place everyone in the same aesthetic framework based on hard-tissue parts may not result in ideal facial beauty because the soft-tissue response is unpredictable. Although a clinician needs to take aesthetics into consideration when treatment-planning, the use of rigid rules may be counterproductive.13 Ideal facial beauty can only be achieved if the analyses of both soft and hard tissues are taken into account. Hence, clinicians need to have basic treatment-planning guidelines that minimize the need for subjective analyses and that use evidence-based, published literature as a starting point.
Clinical Guidelines
The clinical guidelines should be written from the perspective of a surgical and orthodontic team. It is important at this stage to state that ideal facial and dental aesthetics requires a multidisciplinary approach that also involves other team members, including the restorative dentist.
Cephalometric treatment-planning (CTP) from the STC is a process of correcting seven things: 1) maxillary incisor inclination, 2) mandibular incisor inclination, 3) maxillary incisor position (both AP and vertical), 4) proper anterior overbite, 5) proper anterior overjet, 6) occlusal plane adjustment, and 7) genioplasty, if needed.
The maxillary anterior teeth are the starting point of the CTP. The anterior teeth display, as well as the existing upper lip length and projection, are taken into account. Upper lip support can be tested by using a dental mirror in front of the upper incisors; this can quantify the need for incisor/maxillary projection. Adjunct cosmetic procedures that involve lip lengthening or incisor/gingival length changes may also be necessary. The position of the upper incisor is corrected in the CTP, and this is followed by the positioning of the lower incisor; angulation, and proper overbite and overjet with the maxillary incisor. The next step is the adjustment of the maxillomandibular occlusal plane. This step will protect the nasal base from excessive projection and maximize chin projection, as needed. The final step is evaluating the chin projection. If needed, a genioplasty can be performed. The CTP takes the clinician through a step-by-step process of evaluating the soft tissues and the skeleton and dentition that support them, thus reducing subjective bias.
In conclusion, these guidelines enable an optimum balance and harmony to be achieved in both orthodontic and orthognathic treatment. In the authors’ opinion, this can be achieved if subjective bias is held in check by forcing objective assessment through STC and CTP. This permits the clinician to quantify and achieve reliable, repeatable, and beautiful facial results.
Michael J. Gunson, DDS, MD, is a partner in the Center for Corrective Jaw Surgery, a practice strictly limited to facial reconstruction including surgery and research in Santa Barbara, Calif. He can be reached at
G. William Arnett, DDS, FACD, is a partner in the Center for Corrective Jaw Surgery. He is the author of numerous books, including the textbook Facial and Dental Planning for Orthodontists and Oral Surgeons. He teaches at several universities. He can be reached at
Dipak Chudasama, BDS, MSC, MORTH RCS, MBA, is the director of research and an assistant professor at the Jacksonville University School of Orthodontics. He can be reached at
References
- Talass MF, Baker RC. Soft tissue profile changes resulting from retraction of maxillary incisors. Am J Orthod Dentofac Orthop. 1987;91(5):385-394.
- Drobocky OB, Smith RJ. Changes in facial profile during orthodontic treatment with extraction of four first premolars. Am J Orthod Dentofac Orthop. 1989;95(5):220-230.
- Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part I. Am J Orthod Dentofac Orthop. 1993;103(4):299-312.
- Wylie GA, Fish LC, Epker BN. Cephalometrics: a comparison of five analyses currently used in the diagnosis of dentofacial deformities. Int J Adult Orthod Orthog Surg. 1987;2(1):15-36.
- Park YC, Burstone CJ. Soft tissue profile—fallacies of hard tissue standards in treatment planning. Am J Orthod Dentofac Orthop. 1986;90(1):52-62.
- Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part II. Am J Orthod Dentofac Orthop. 1993;103(5):395-411.
- Legan HL, Burstone CJ. Soft tissue cephalometric analysis for orthognathic surgery. J Oral Surg. 1980;38:744-751.
- Spradley FL, Jacobs JD, Crowe DP. Assessment of the antero-posterior soft-tissue contour of the lower facial third in the ideal young adult. Am J Orthod. 1981;79:316-325
- Holdaway RA. A soft-tissue cephalometric analysis and its use in orthodontic treatment planning. Part I. Am J Orthod. 1983;84(1):1-28.
- Holdaway RA. A soft-tissue cephalometric analysis and its use in orthodontic treatment planning. Part II. Am J Orthod. 1984;85:279-293.
- Arnett GW, Jelic JS, Kim J, et al. Soft tissue cephalometric analysis: Diagnosis and treatment planning of dentofacial deformity. Am J Orthod Dentofacial Orthop. 1999;116:239-253.
- Arnett GW, RP McLaughlin. Facial and Dental Planning for Orthodontists and Oral Surgeons. London, Mosby/Elsevier. January, 2004.
- Sarver DM, Ackerman JL. Orthodontics about face: The re-emergence of the aesthetic paradigm. Am J Orthod Dentofac Orthop. 2000:117:575-576.









