by James J. Hilgers, DDS, MS
An update on noncompliance treatment
For years, orthodontists have been aware of the need for control of their treatment mechanics. Without control, the chance of achieving a quality result is virtually nil. The problem is that, even without optimal patient cooperation, we are still charged with producing an ideal result. As society changes, many patients are becoming less responsible for their outcomes and more dependent on us to do the job for them.
It is frustrating; but still, it is reality. Methods of reducing the need for compliance are growing exponentially, and many of them offer excellent potential. I think most orthodontists are aware of bone screws, even though they may not be using them yet. This article is not so much about how to achieve a Class I molar relationship, but more about how to maintain that gain with anchorage control, whether the clinician is using a pendulum, a Herbst appliance, bone screws, a distal jet, or the myriad other forms of noncompliance treatment.
Case Selection is Key
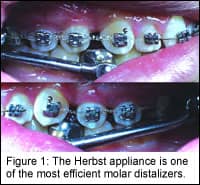
The Herbst and Molar Distalization
Much has been published about what a Herbst appliance can and cannot do. One thing seems to be fairly clear: It doesn’t grow the mandible. Just because the Herbst appliance doesn’t grow the mandible does not, however, mean that it is not a superb appliance for Class II correction. Avoiding the Herbst because it doesn’t produce profound growth changes is ignoring some of the marvelous functional and tooth-moving capacity of the Herbst appliance. The question is, how do we use a Herbst appliance and harness some of these significant changes? Without a doubt, the Herbst is one of the most efficient molar distalizers we know about (because it is so slow and methodical); and in conjunction with its prolific functional changes, we can use the techniques described here to harness this molar distalization in a most predictable manner (Figure 1).
Rapid Palatal Expansion and Molar Distalization
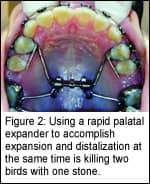
Secure Anchorage Maintenance
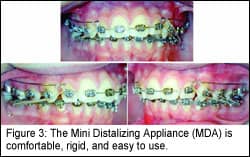  |
There are various methods of molar anchorage (and I have used many), but the simplest seems to be the best. A secure anchorage system should:
1) be immediate—the moment the distalizer is removed;
2) be totally stable;
3) initiate molar control, including distorotation and uprighting; and
4) allow for unencumbered distal floating of the buccal segments.
I have found that the most effective way of accomplishing all these objectives is to place an upper utility arch that uses the four anterior teeth to provide anchorage. It is easy to place and provides a method of using Class II elastics early in treatment. A preformed adjustable utility arch has worked well for this purpose. This unique archwire has an anterior segment of .016 x .016 NiTi to allow easy alignment of crowded incisors; a rigid .016 x .016 stainless steel posterior segment for molar control; and an adjustable buccal sleeve to unite each segment and ensure that several preformed sizes will fit virtually any case.
The lower arch should be bonded, leveled and aligned as early in the treatment sequence as possible. It is important to get a large and rigid lower archwire to bear Class II elastics. In a .018 slot, this archwire is usually a .016 x .022 TMA. As the upper molars are distalized, there is usually a transient opening of the bite, clearing the lower arch for bonding. Since many of the types of malocclusions selected for distalization are Class II, Division II in nature, this clearing of the lower arch may take several months.
Passive Free Floating
Attempts to close spaces too quickly in the upper buccal segments created by molar distalization are usually fraught with problems. They can aggravate or create an anterior open bite, bring the upper molar back into a Class II position, and tip the upper incisors forward. This is the time for patience. I have found that if the upper buccal segments are allowed to float distally (due to the pressure of trans-septal fibers), 75% of the residual spaces will close spontaneously without further straining anchorage. This is referred to as passive free floating and can take from 3 to 6 months, depending upon overtreatment of the molar position and the amount of space to be closed. While passive free floating is under way, no attempt to align or work out rotations in the buccal is done. Alignment and consolidation of the upper arch will occur later. The focus is on maintaining an overcorrected molar position to avoid “round-tripping” the case. In this 3- to 6-month period, the lower arch can often be aligned sufficiently to place a lower rigid or ideal edgewise wire.
When to Use Class II Elastics (or Fixed Class II Springs)
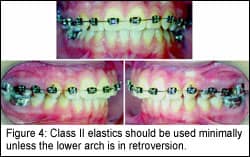
Class II elastics can be used as soon as a lower ideal archwire is placed. This can be very early in the treatment sequence. It is not unusual to start light Class II elastics while the upper distalizing appliance is still in place. Early Class II elastics help avoid incisor flaring and can aid in maintaining overjet at this time in treatment. Applying Class II elastics is a strain on the lower arch, so they should be used minimally, unless the lower arch is in retroversion (Figure 4).
Active Free Floating
Once most of the spaces in the buccal segments have closed spontaneously (and without the friction associated with sliding mechanics on an archwire), the small residual spaces can be closed using active free floating. With the upper utility arch still in place, very light elastomeric chain or elastic thread is extended from the molar to the buccal segment teeth. Monitoring this residual space closure is very important, because it will occur rapidly.
If active free floating is used, the patient should typically be seen on two-week intervals. In most cases, the space closure will occur at the two-week interval. Class II elastics are attached to the upper utility archwire to maintain anchorage (unless the molars are so overcorrected that this is not needed). The space created by distalizing the upper molars has now been moved entirely to the mesial of the upper cuspids. The buccal segments have been corrected. The anterior segment has not.
Leveling and Alignment of the Upper Arch
At this stage in treatment, the center of attention should be aligning and leveling the upper arch. Prior to this time, segmental treatment has dominated. The patient can now be seen at 8-week intervals while a series of leveling archwires are placed. There is a concentration on rotations and root paralleling. No attempt is made to close the large spaces between the anterior and posterior buccal segments until the integrity of the upper arch is established.
Retraction of Anterior Teeth
The last component of noncompliance treatment is to retract and torque (or detorque) the upper incisors. If there is still a residual deep bite caused by the upper incisors, an asymmetrical “T” loop archwire is used to accomplish these movements. This is the most common method of anterior retraction, but a simple closing archwire is used if it will suffice. You should be at the finishing stage of treatment at this point, since minimal Class II elastics were used at an early point in the treatment cycle.
Summary
Orthodontics has sometimes been referred to as a “5 mm specialty.” This means that most cases can be corrected by moving the teeth five millimeters or less. So it is with most noncompliance therapy. Most molars only need to be moved distally a few millimeters to achieve a Class I relation.
The key to treatment is to judiciously hold that corrected molar position. By doing so, most gross reduction of the malocclusions can be accomplished in less than 1 year. Early and rapid reduction of the malocclusion gives you time to finish. You shouldn’t be spending the last 6 months of treatment pleading for compliance to correct the remnants of the Class II malocclusion. This often leads to compromise, frustration, and lengthy treatment times. When you use your noncompliance appliance of choice, don’t let the cat out of the bag once you’ve established molar position.
James J. Hilgers, DMD, MS, has published more than 90 articles in scientific and clinical journals. He is an assistant clinical professor at Loma Linda University, and has a private practice in Mission Viejo, Calif. He can be reached at [email protected].