by Derek Mahony, BDS, MScOrtho
Refining occlusion with muscle balance to enhance long-term orthodontic stability
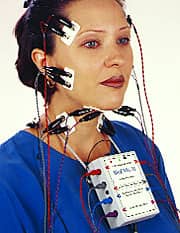
Muscle Balance and Occlusion
Many well-respected orthodontists agree that there is more to occlusion than just teeth. Temporomandibular (TM) joint function and the maxillo-mandibular relation are as much a part of occlusion as are the teeth. Consequently, when a malfunction occurs within the TM joints or a maxillo-mandibular mal-relation exists, a compensatory response is elicited from the stomatognathic musculature. Most often, that response can be measured through electromyography (EMG).
More than 50 years ago, one orthodontist began to record muscle activity through surface EMG in an effort to better understand the functions of the muscles of mastication.1 In the years since, surface EMG has revealed several key facts about the relationship between the muscles and a patient’s occlusion. Today, we can routinely record up to eight channels of EMG data right in the clinic (Figure 1), and data interpretation can lead us to a better understanding of our patient’s specific condition.
In Figure 2, we see muscles that are: a) relaxed at rest (the normal condition); b) hyperactive at rest (indicating a maxillo-mandibular mal-relation); and 3) exhibiting a neurological abnormality (large motor-unit firing). While these factors routinely go unmeasured, their contribution to a precise diagnosis can be highly significant, even to the long-term outcome of a particular case.2-5
Determining muscle balance in function using an EMG is an easy task.6-13 Typically, the patient is asked to clench in maximum intercuspation and then swallow. The clench will appear balanced (Figure 3a) or unbalanced (Figure 3b). The swallow will either be with the teeth together (Figure 3c) or with a tongue-thrust (Figure 3d). Then, if an appliance is used, muscle activity can be recorded before, during, and after adjustment of the appliance. This will immediately demonstrate the effectiveness of the appliance.14-20
If we see that the muscles are balanced, we know we have a result that will remain stable. But, if the muscles are not in balance, we cannot tell from the EMG recordings alone exactly what to do about it. While much has been learned about muscle hyperactivity and the various conditions of imbalance that can exist within the masticatory musculature, EMG is not, nor will it likely ever be, adequate to the task of directing case treatment by itself. While surface EMG is a fast, easy, and reliable way to record the relative contraction levels of the muscles at rest or in function, it has a low sensitivity to occlusal-force locations and the timing of tooth contacts.
Using an Electronic Occlusal Wafer
The simplest solution to the problem of evaluating the timing and force of occlusal contacts is to use an electronic occlusal wafer.21-23 It provides a very sensitive measure of contact force and a moving picture of the order in which the contacts occur.24-32 It is the only technology available to the clinician that can show precisely the order in which contacts occur and, simultaneously, the relative force of each distinct contact. The new high-density sensors are flexible, more precise, and very durable (usable for up to 30 registrations).
A bite-force recording is taken by having the patient bite down several times on the electronic occlusal wafer to condition it. This allows it to conform to the shape of the arch. Then, a recording is taken with the patient closing from rest position into the intercuspal position, followed by a clench. Other recordings can also be taken in centric relation, lateral excursions. and protrusion.
In the recording in Figure 4, the initial contact points occur only on the incisors. As the patient continues to close, a contact appears on the right area of the second molar. Eventually, a contact appears on the left second molar, creating a tripod effect.
When the recording is replayed as a “force movie,” a 3-D graph is displayed showing the relative force at each point of contact (Figure 5). Again, we see that the initial contacts are on the incisors, the next are on the right posterior, and the last are on the left second molars. What is also evident is that in full closure, the highest-contact force is actually on the left second molar (indicated by the tallest spike), despite the lateness of the contact. Further inspection clearly suggests that the reason the excessive force is being borne by the left second molar is due to a lack of solid contacts on the left first molar and bicuspids. In spite of the large number of contact points around the arch, this is an occlusion badly in need of adjustment.
As we analyze the tracing above, though the picture of occlusion of this case is clear, we realize that we do not and cannot, from this information, understand what the musculature is doing to accommodate. But there is a way to do both.
Electronic Occlusal Wafer and EMG
In previous studies, attempts have been made to correlate electronic occlusal wafer data with EMG data.33,34 Recently, the two companies who separately manufacture the two machines have reached a milestone by making their programs talk to one another.35 This is not something that happens often in dentistry, but the synergy created now offers a unique opportunity for dentists to more clearly and comprehensively understand their patients’ occlusal conditions. The reason that the programs needed to talk to one another was to synchronize their respective data streams. This is accomplished by having either program act as a “master” while the other program acts as a “slave” to it. That is, a dentist can run the electronic occlusal wafer program, and the EMG program will dutifully “follow” it, or vice versa. This is true in recording as well as in playback analysis.
Analyzing the Combined Traces
When we see that the highest force of contact is on the left, can we assume that the greatest muscle activity will be the same? Not at all. Figure 6 shows an example of a patient with a higher force level on the left side (63% of the total), focused in the bicuspid area. At the same time, we clearly see that the right anterior temporalis is firing at nearly twice the level of the left one. It is also apparent that the combined activities of the right masseter and temporalis are far greater than the same muscles on the left. How is this possible?
Not one of the muscles of mastication that elevates the mandible is positioned such that there is a straight vertical relationship between the origin and the insertion. Each elevator muscle has a horizontal component to its direction of applied force. Due to the ginglymo-arthroidial structure of the temporomandibular joints, the mandible is able to move freely forward and back, left, and right. The same “elevator muscles” that apply vertical forces can and do apply horizontal forces to the mandible as needed for function. In Figure 7 (page 44), then, we can see that, while the left-side muscles are applying more force in the vertical direction, the right-side temporalis must be applying a significant amount of its force in a horizontal direction. However, with some extra effort, it is possible to achieve a muscle- and force-balanced occlusion.
Balanced Forces Do Not Guarantee Balanced Muscles
Sometimes, we can record a relatively even balance of forces between the right and left sides, but the patient is still not comfortable. Even with adequate stable contacts on both sides, some patients still complain. The patient in Figure 8 had regular temporal headaches. The left-right force balance was rather good at 56% right to 44% left. It is evident that the initial contact is on the left side (see the center of the force vector) and that, during the closure, the force passes to the right side before reaching its balanced force condition at maximum intercuspation. However, notice that the temporalis muscles are contracting at 21¼2 times greater levels than the masseter muscles. Soon after a repositioning appliance was placed that balanced both the muscle and the forces, the headaches were relieved.
With the technology that is available today, an ordinary practicing orthodontist has the ability to more thoroughly evaluate the masticatory system than ever before. It is now possible to routinely adjust an occlusion, not only to equalize the occlusal forces, but also to create an environment where the muscles can function in harmony with one another. z
Derek Mahony, BDS, MScOrtho, has been a keynote speaker at the International Orthodontic Summit meetings, the International Association of Orthodontics meetings, and the American Association of Functional Orthodontics meetings. He can be reached at [email protected].
References
1. Thompson JR. Concepts regarding the function of the stomatognathic system. J Am Dent Assoc. 1954;48:626–637.
2. Gervais RO, Fitzsimmons GW, Thomas NR. Masseter and temporalis electromyographic activity in asymptomatic, subclinical, and temporomandibular joint dysfunction patients. Cranio. 1989;7(1):52–527.
3. Glaros AG, McGlynn FD, Kapel L. Sensitivity, specificity, and the predictive value of facial electromyographic data in diagnosing myofascial pain-dysfunction. Cranio. 1989;7(3):189–193.
4. Glaros AG, Glass EG, Brockman D. Electromyographic data from TMD patients with myofascial pain and from matched control subjects: evidence for statistical, not clinical, significance. J Orofac Pain. 1997;11(2):125–129.
5. Kamyszek G, Ketcham R, Garcia R Jr, Radke J. Electromyographic evidence of reduced muscle activity when ULF-TENS is applied to the Vth and VIIth cranial nerves. Cranio. 2001;19(3):162–168.
6. Belser UC, Hannam AG. The influence of altered working-side occlusal guidance on masticatory muscles and related jaw movement. J Prosthet Dent. 1985;53(3):406–413.
7. McCarroll RS, Naeije M, Hansson TL. Balance in masticatory muscle activity during natural chewing and submaximal clenching. J Oral Rehabil. 1989;16(5):441–446.
8. Visser A, McCarroll RS, Oosting J, Naeije M. Masticatory electromyographic activity in healthy young adults and myogenous craniomandibular disorder patients. J Oral Rehabil. 1994;21(1):67–76.
9. Christensen LV, Rassouli NM. Experimental occlusal interferences. Part I. A review. J Oral Rehabil. 1995;22(7):515–520.
10. Christensen LV, Rassouli NM. Experimental occlusal interferences. Part II. Masseteric EMG responses to an intercuspal interference. J Oral Rehabil. 1995;22(7):521–531.
11. Borromeo GL, Suvinen TI, Reade PC. A comparison of the effects of group function and canine guidance interocclusal device on masseter muscle electromyographic activity in normal subjects. J Prosthet Dent. 1995;74(2):174–180.
12. Christensen LV, Mohamed SE. Bilateral masseteric contractile activity in unilateral gum chewing: differential calculus. J Oral Rehabil. 1996;23(9):638–647.
13. Saifuddin M, Miyamoto K, Ueda HM, Shikata N, Tanne K. An electromyographic evaluation of the bilateral symmetry and nature of masticatory muscle activity in jaw deformity patients during normal daily activities. J Oral Rehabil. 2003;30(6):578–586.
14. McCarroll RS, Naeije M, Kim YK, Hansson TL. Short-term effect of a stabilization splint on the asymmetry of submaximal masticatory muscle activity. J Oral Rehabil. 1989;16(2):171–176.
15. Naeije M, Hansson TL. Short-term effect of the stabilization appliance on masticatory muscle activity in myogenous craniomandibular disorder patients. J Craniomandib Disord. 1991;5(4):245–250.
16. Lobbezoo F, van der Glas HW, van Kampen FM, Bosman F. The effect of an occlusal stabilization splint and the mode of visual feedback on the activity balance between jaw-elevator muscles during isometric contraction. J Dent Res. 1993;72(5):876–882. Erratum in: J Dent Res 1993;72(8):1264.
17. Visser A, Naeije M, Hansson TL. The temporal/masseter co-contraction: an electromyographic and clinical evaluation of short-term stabilization splint therapy in myogenous CMD patients. J Oral Rehabil. 1995;22(5):387–389.
18. al-Quran FA, Lyons MF. The immediate effect of hard and soft splints on the EMG activity of the masseter and temporalis muscles. J Oral Rehabil. 1999;26(7):559–563.
19. Ferrario VF, Sforza C, Tartaglia GM, Dellavia C. Immediate effect of a stabilization splint on masticatory muscle activity in temporomandibular disorder patients. J Oral Rehabil. 2002;29(9):810–815.
20. Roark AL, Glaros AG, O’Mahony AM. Effects of interocclusal appliances on EMG activity during parafunctional tooth contact. J Oral Rehabil. 2003;30(6):573–577.
21. Maness WL, Podoloff R. Distribution of occlusal contacts in maximum intercuspation. J Prosthet Dent. 1989;62(2):238–242.
22. Maness WL. Laboratory comparison of three occlusal registration methods for identification of induced interceptive contacts. J Prosthet Dent. 1991;65(4):483–487.
23. Reza Moini M, Neff PA. Reproducibility of occlusal contacts utilizing a computerized instrument. Quintessence Int. 1991;22(5):357–360.
24. Mizui M, Nabeshima F, Tosa J, Tanaka M, Kawazoe T. Quantitative analysis of occlusal balance in intercuspal position using the T-Scan system. Int J Prosthodont. 1994;7(1):62–71.
25. Gonzalez Sequeros O, Garrido Garcia VC, Garcia Cartagena A. Study of occlusal contact variability within individuals in a position of maximum intercuspation using the T-SCAN system. J Oral Rehabil. 1997;24(4):287–290.
26. Garcia Cartagena A, Gonzalez Sequeros O, Garrido Garcia VC. Analysis of two methods for occlusal contact registration with the T-Scan system. J Oral Rehabil. 1997;24(6):426–432.
27. Suda S, Matsugishi K, Seki Y et al. A multiparametric analysis of occlusal and periodontal jaw reflex characteristics in young adults with normal occlusion. J Oral Rehabil. 1997;24(8):610–613.
28. Garrido Garcia VC, Garcia Cartagena A, Gonzalez Sequeros O. Evaluation of occlusal contacts in maximum intercuspation using the T-Scan system. J Oral Rehabil. 1997;24(12):899–903.
29. Kirveskari P. Assessment of occlusal stability by measuring contact time and centric slide. J Oral Rehabil. 1999;26(10):763–766.
30. Kerstein RB. Improving the delivery of a fixed bridge. Dent Today. 1999;18(5):82-4, 86–87.
31. Suda S, MacHida N, Momose M et al. A multiparametric analysis of occlusal and periodontal jaw reflex characteristics in adult skeletal mandibular protrusion before and after orthognathic surgery. J Oral Rehabil. 1999;26(8):686–690.
32. Saracoglu A, Ozpinar B. In vivo and in vitro evaluation of occlusal indicator sensitivity. J Prosthet Dent. 2002;88(5):522–526. Comment in: J Prosthet Dent. 2003;90(3):310; author reply 310–311.
33. Kerstein RB, Wright NR. Electromyographic and computer analyses of patients suffering from chronic myofascial pain-dysfunction syndrome: before and after treatment with immediate complete anterior guidance development. J Prosthet Dent. 1991;66(5):677–686. Comment in: J Prosthet Dent. 1993;70(1):99–100.
34. Hidaka O, Iwasaki M, Saito M, Morimoto T. Influence of clenching intensity on bite force balance, occlusal contact area, and average bite pressure. J Dent Res. 1999;78(7):1336–1344.
35. Kerstein RB. Combining technologies: A computerized occlusal system synchronized with a computerized electromyograhic system. Cranio. 2004;22(2):96–109.
Why the Electronic Occlusal Wafer, at 85 Microns, Is Not Too Thick
According to the latest research on mandibular function (Gallo et al), we now know that the sagittal path of closure is more complicated than a simple hinge movement. In fact, the “helical axis of rotation” moves from the vicinity of the angle of the mandible (early in opening) to about midramus (late in opening) in close proximity to where the inferior alveolar nerve enters the mandibular foramen. For a voluntary closure between rest and occlusion (2–3 mm), the average amount of rotation has been measured at 0.7º (Lewin A and Moss C). For an 85-micron change, that is about 0.02° of rotation (about 1.5 minutes of arc). If the A/P distance between the incisors and the second molars is 40 mm, 1.5 minutes of arc translates to an 18-micron difference in vertical change (more in the anterior, less in the posterior) between “wafer in” and “wafer out.” This is a very small difference in comparison to the size of an occlusal adjustment being made, and it is well within the adaptive capacity of the system. Another benefit of placing the electronic occlusal wafer between the arches is that it reduces the acuity of proprioception, which reduces, but does not eliminate, the ability of the central nervous system to avoid any existing prematurities.
—DM