by Laurance Jerrold, DDS, JD, and Nona Naghavi, DDS
Techniques for preventing and reversing aesthetic damage caused by demineralization
No matter how advanced the materials and techniques used in dentistry have become, the development of white spot lesions around orthodontic brackets still remains a big problem.

Prevalence
It has been shown that there is a significant increase in the prevalence and severity of demineralization in subjects who undergo orthodontic treatment compared to those who do not.1,2 White spot lesions have been reported to have a prevalence of 2% to 96% in orthodontic patients.3-7 Nearly half of all orthodontic patients have visible white spot lesions while in treatment. These lesions can last up to 2 years.8 Also of concern is the possibility that the prevalence of smooth surface lesions can increase by up to 50% during treatment.3,9 Ogaard and colleagues found more lesions occurring on molars than on incisors, but this could be due to the fact that in their study all molars were banded as opposed to bonded. In banded molars, a small breakdown of the cement layer can lead to leakage and demineralization. A high prevalence of white spot lesions was also seen on lower premolars, canines, and upper lateral incisors. Brackets are typically placed more gingivally in these areas, leading to more plaque buildup; thus the higher prevalence.
Etiology
The main etiologic factors for white spot lesions are tooth location and morphology, dental biofilm organisms, fermentable carbohydrates in the diet, and saliva flow rate and composition. The bracket, band, and wire surfaces are not smooth, and they create plaque trap areas that, when combined with difficult tooth cleaning and limited self-cleansing mechanisms, encourage the accumulation of aciduric bacteria such as Streptococcus mutans and Lactobacilli. The presence of fermentable carbohydrates in patients’ diets completes this cycle, leading to the demineralization of enamel. There is an almost linear correlation between plaque accumulation and white spot lesions around orthodontic brackets.10 These lesions can be an aesthetic problem even 5 years after the end of orthodontic treatment,1 and because they can be irreversible, it is important to discuss this with the patient and be familiar with available preventive measures.11
Prevention
Some caries prevention strategies include fluoride (delivered by a professional or at home), salivary stimulation (whether through chewing gum or pharmacological means), diet modification, and antimicrobial and remineralizing agents. It has been shown that fluoride mouth rinse and regular use of fluoride toothpaste may prevent lesion formation around brackets.12 Fluoride helps prevent demineralization and aids remineralization by becoming incorporated in the crystalline lattice of the enamel hydroxyapatite structure, ultimately rendering it more acid-resistant.
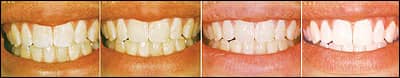
The appearance of the teeth can be significantly improved using a protocol with etching and MI Paste. Images courtesy of Lori Laughter, RDH.
A recent product of interest introduced by GC America is MI Paste™, which contains RECALDENT™, a complex of Casein Phosphopeptide (CPP) and Amorphous Calcium Phosphate (ACP). The casein in CPP is obtained from cow’s milk and forms a new compound with ACP. CPP-ACP is bioavailable and releases calcium and phosphate. It has been shown to help remineralize subsurface lesions in in situ testing.13 CPP-ACP is also found in chewing gum (Trident Xtra Care™, Cadbury Adams). RECALDENT is found only in MI Paste™and Trident Xtra Care.
This product has been widely used in orthodontic practices to help prevent the development of white spot lesions and has been shown to help harden enamel13-15 and inhibit the progression of subsurface lesions in enamel.16 Its modes of action are the following:
- delivering supercharged calcium and phosphate ions to enamel and dental plaque to a level of supersaturation, thereby enhancing remineralization;
- buffering the oral cavity acids; and
- prevention and reversal of already existing early carious lesions.17
Any incipient lesions can be treated locally with this topical tooth cream to help achieve subsurface remineralization in a relatively short period of time. It has also been said that CPP-ACP, once incorporated into dental plaque, can result in the formation of less cariogenic plaque.7 Because CPP-ACP is a milk-derived protein (capitalizing on the anticavity properties of milk), patients with a milk protein allergy should not use this material. Patients can use CPP-ACP if they are lactose intolerant, since the lactose content is less than 0.01%. Some studies have shown that the role of CPP-ACP in caries reduction could be supplementary to the effects of topical fluoride.2,17
Clinical Application
In patients without fixed orthodontic appliances, MI Paste can be smeared over all surfaces in the oral cavity using one’s tongue and a clean finger, and left to dissolve overnight. It also works in combination with fluoride. There is no need to etch prior to application of the paste in active carious lesions. Arrested lesions can be etched for 15 seconds so that the surface becomes more porous and permeable.
In orthodontic patients with braces, the paste should be applied twice daily to prevent plaque accumulation around brackets and archwires. In addition, the paste can be applied at the debond visit to maintain the reflectivity of the surfaces. This is done after all the resin is removed from the enamel surfaces, followed by gentle microabrasion. The patient continues to apply the paste once a day for a few weeks. MI Paste can also be used for the reversal of white spots,18 using a protocol involving microabrasion or etching which has been found to improve the appearance of white spots,19 followed by the use of the cream.
Suggested White Spot Reversal Protocol
- Take photos of white spot lesions prior to the start and at the conclusion of treatment.
- It is important not to overetch the tooth surface. Pay careful attention to the etching material, the concentration, and application time. Some clinicians prefer to pumice first, then etch.
- Apply 35% to 37% phosphoric acid gel to the white spot lesions and leave it for 15 to 30 seconds, and no longer than 1 minute. Be conservative when etching; you can always re-etch if necessary, then rinse.
- Apply the etching material on the white spot lesion being treated, not the entire tooth surface.
- For microabrasion, gently pumice for 15 to 30 seconds, using nonfluoridated, nonglycerin pumice such as “Flour of Pumice,” then rinse.
- Dry the tooth and review the effect. Sometimes you may have to re-etch/pumice. The tooth will appear frosty.
- For in-office use, we suggest using a prophy cup to apply MI Paste; for at-home application, the patient can use a finger or a cotton tip.
- Apply a layer of MI Paste on the etched tooth surfaces. Leave on the tooth surface for a minimum of 5 minutes. You can leave the paste on the tooth surface longer to maximize the uptake of calcium and phosphate.
- Advise patients not to eat or drink for 30 minutes, maximizing the uptake of calcium and phosphate into the dentinal tubules.
- Instruct patients to apply paste twice daily for a minimum of 5 minutes; using a custom tray is optional.
- We suggest refraining from ingesting staining products during the white spot reversal procedure. After etching, the dental tubules are wide open and can easily pick up stains. Therefore, no wine, tea, coffee, cola drinks, grape juice, tomato sauces, or smoking.
- Have the patient return for evaluation in 7 to 10 days. Repeat the above procedures if necessary.
Laurance Jerrold, DDS, JD, is the president of Orthodontic Consulting Group LLC, Jacksonville, Fla. He can be reached at
Nona Naghavi, DDS, is a first-year resident at the Jacksonville University School of Orthodontics. She can be reached at
References
- Ogaard B. Prevalence of white spot lesions in 19-year-olds: A study on untreated and orthodontically treated persons 5 years after treatment. Am J Orthod Dentofacial Orthop. 1989;96:423-427.
- Sudjalim TR, Woods MG, Manton DJ, et al. Prevention of demineralization around orthodontic brackets in vitro. Am J Orthod Dentofacial Orthop. 2007;131:705,e1-705.e9.
- Gorelick L, Geiger AM, Gwinnett AJ. Incidence of white spot formation after bonding and banding. Am J Orthod. 1982;81:93-98.
- Mizrahi E. Enamel demineralization following orthodontic treatment. Am J Orthod. 1982;82:62-7.
- Ogaard B, Rolla G, Arends J, ten Cate JM. Orthodontic appliances and enamel demineralization. Part 2. Prevention and treatment of lesions. Am J Orthod Dentofacial Orthop. 1988;94:1238.
- Mitchell L. Decalcification during orthodontic treatment with fixed appliances-an overview. Br J Orthod. 1992;19:199-205.
- Rose RK. Binding characteristics of streptococcus mutans for calcium and casein phosphopeptide. Caries Res. 2000;34:427-431.
- Basdra EK, Huber H, Komposch G. Fluoride release from orthodontic bonding agents alters the enamel surface and inhibits enamel demineralization in vitro. Am J Orthod Dentofacial Orthop. 1996;109:466-472.
- Mizrahi E. Surface distribution of enamel opacities following orthodontic treatment. Am J Orthod. 1983;84:323-331.
- Zachrisson BU, Zachrisson S. Caries incidence and orthodontic treatment with fixed appliances. Scand J Dent Res. 1971;79:183-92.
- Gorton J, Featherstone JDB. In vivo inhibition of demineralization around orthodontic brackets. Am J Orthod Dentofacial Orthop. 2003;123:10-14.
- O’Reilly MM, Featherstone JDB. Demineralization and remineralization around orthodontic appliances: an in vivo study. Am J Orthod Dentofacial Orthop. 1987;92:33-40.
- Cai F, Shen P, Walker GD, et al. Remineralization of enamel subsurface lesions by chewing gum with added calcium. J Dent. 2009;37(10):763-768.
- Tantbirojn D, Huang A, Ericson MD, Poolthong S. Change in surface hardness of enamel by a cola drink and a CPP-ACP paste. J Dentistry. 2008;36(1):74-79.
- Pai D, Bhat SS, Taranath A, Sargod S, Pai VM. Use of laser fluorescence and scanning electron microscope to evaluate remineralization of incipient enamel lesions remineralized by topical application of casein phosphopeptide amorphous calcium phosphate (CPP-aCP) containing cream. J Clin Pediatr Dent. 2008;32(3):201-6.
- Walker GD, Cai F, Shen P, et al. Casein phosphopeptide-amorphous calcium phosphate incorporated into sugar confections inhibits the progression of enamel subsurface lesions in situ. Caries Res. 2010;44(1):33-40.
- Reynolds EC, CAi F, Cochrane NJ, et al. Fluoride and casein phosphopeptide-amorphous calcium phosphate. J Dent Res. 2008;87(4):344-348.
- Bailey DL, Adams GG, Tsao CE et al. Regression of post-orthodontic lesions by a remineralizing cream. J Dent Res. 2009;88(12):1148-1153.
- Willmot D. White spot lesions after orthodontic treatment. Semin Orthod. 2008;14:209-219.









