by Leslie Canham, CDA, RDA
Infection-control procedures before, during, and after the placement of temporary anchorage devices
 |
| Leslie Canham, CDA, RDA |
The hot topic in orthodontics today is temporary anchorage devices (TADs). Other names for these devices are miniscrews, microscrews, mini-implants, and temporary orthodontic implants. TADs are used by orthodontists to move teeth in the desired direction without moving adjacent teeth. They are small screws made from titanium alloy that are drilled into the alveolar process as anchorage units. The placement of a TAD is a simple surgical procedure that may be performed in the orthodontic office, as long as infection-control and safety protocols are followed.
TADs can be placed painlessly with the use of local anesthesia and are removed after they have completed their task. The benefits to the patient include a shorter treatment period and not having to comply with using other devices.
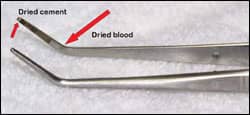
John W. Graham, DDS, MD, an orthodontist who has placed hundreds of TADs, says, “Patients should have a thorough understanding of how the miniscrew may benefit them. The orthodontist needs to be clear about why the miniscrew is being utilized, and also needs to be explicit about how painless the insertion of a miniscrew really is. I recommend that the doctor have a miniscrew placed in himself/herself at a miniscrew course, and have photographs taken of the miniscrew in place. Then, the photograph may be used during consultations or chairside to demonstrate that the doctor truly has firsthand experience as a miniscrew recipient.”
 |
In the past, orthodontists would refer patients to an oral surgeon to place implants. Today, many orthodontists are placing TADs in their own offices. This saves the patient time and money, and ensures that the TAD will be placed exactly where the orthodontist wants it. Since the orthodontist is now performing a surgical procedure, the orthodontic assistant must deal with greater occupational hazards. This new procedure calls for a better understanding of infection control and safety.
TAD Training
 |
To help meet the new challenges, orthodontic assistants need additional training. The Occupational Health and Safety Administration (OSHA) requires that initial training be provided to all employees before they perform tasks that could expose them to infectious agents. This training should include techniques to prevent contact with infectious agents, instrument-processing protocols, and how personal protective attire is used. The training must be repeated when tasks, such as the use of anesthetic needles, are introduced that might expose the orthodontic assistant to new hazards. The training must be site-specific and include information on the office-exposure control plan.
The exposure-control plan is a written plan that requires the employer to identify which individuals have occupational exposure and who will receive training, protective equipment, vaccinations, and other protections as stated in the Bloodborne Pathogen Standard. An effective exposure-control plan is designed to eliminate or minimize employee exposure to bloodborne pathogen hazards in the workplace. The exposure-control plan must have a section about exposure incidents. An exposure incident involves contact between blood or other potentially infectious materials and the eye, mouth, other mucous membrane, nonintact skin, or parenteral under the skin (otherwise known as a needlestick).
When an exposure incident occurs, immediate action must be taken to ensure compliance with the OSHA Bloodborne Pathogen Standard and to expedite medical treatment for the exposed individual. OSHA requires that bloodborne pathogen training be provided at least annually, at no charge to employees, and include a review of the office exposure-control plan. Employees must have an opportunity to ask questions of the person conducting the training, and the training must be documented.
Before introducing TAD placement to the orthodontic practice, conduct updated training on basic infection-control policies and procedures. Placement of TADs is considered an invasive procedure because the implant penetrates soft tissue and contacts bone. Infection control for orthodontic practices now includes procedures for aseptic use of critical instruments.
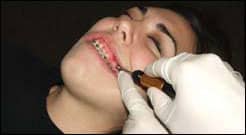 |
| The assistant must maintain a sterile field while the implant procedure is being performed. |
TAD-Placement Hygiene
Before the orthodontist performs implant procedures, the orthodontic assistant must prepare the treatment area by cleaning and disinfecting all clinical contact surfaces with an FDA-registered intermediate-level disinfectant that has a tuberculocidal kill claim. Clean barriers should be placed where applicable. After routine hand hygiene has been performed, the assistant should don gloves and set up the treatment area by placing the closed sterile implant package and the sterile instrument bag or cassette on the treatment tray or cart. Both containers should remain closed until the patient is prepared for the procedure and the orthodontist and assistant are ready to begin treatment.
The next step is to don gowns, surgical face masks, and protective eyewear. Then, perform appropriate hand-hygiene procedures. Hand hygiene is considered the single most critical measure for reducing the risk of transmitting organisms to patients. For routine dental examinations and nonsurgical procedures, handwashing and hand antisepsis can be achieved using either plain or antimicrobial soap and water. Placement of TADs would upgrade the hand-hygiene protocol to surgical hand antisepsis, which eliminates transient flora and reduces resident flora for the duration of the procedure to prevent introduction of organisms in the operative wound if gloves become punctured or torn. Skin bacteria can rapidly multiply under surgical gloves if hands are washed with soap that is not antimicrobial. Thus, an antimicrobial soap or alcohol hand rub with persistent activity should be used before surgical procedures.1
After you have performed appropriate hand hygiene procedures and put on gloves, you can open the sterile treatment tray. A typical treatment tray might include a mirror, a syringe, cotton rolls, miniscrew attachments (nonsterile), cotton forceps, 2×2 gauze, a sterile tissue punch, a sterilized screwdriver, and any other necessary items. Prepackaged orthodontic miniscrews are presterilized. If the miniscrews come nonsterile, then I recommend autoclaving them with spore testing.
Prior to performing the procedure, instruct the patient to rinse with chlorhexidine to disinfect the insertion area. The assistant must maintain a sterile field while the implant procedure is being performed. This includes not touching the implant itself prior to placement. If the implant is dropped onto a nonsterile surface, it must be resterilized. Because all implantable devices should be quarantined after sterilization until the results of biological monitoring are known, unwrapped or flash sterilization of implantable items is not recommended.
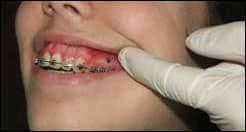 |
| After placement of the TAD, the syringe needle should be removed from the syringe and placed in the sharps container. |
TAD Cleanup Hygiene
After placement of the TAD, the syringe needle should be removed from the syringe and placed in the sharps container. The contaminated instruments should be transported in a closed container or on a tray to the sterilization area. The orthodontic assistant should put on puncture-resistant utility gloves and place the contaminated instruments in the ultrasonic tank or instrument washer. If manual scrubbing is performed, a long-handled brush should be used. Instruments should then be rinsed and inspected for any remaining debris. Once instruments have been dried and packaged or wrapped, they are ready for loading in the sterilizer. After instruments have been sterilized, inspect the instruments packs to ensure that they have not been compromised by instrument pokes or tears. Also, check that the pack’s chemical indicator has changed color, indicating that it has been processed. Instruments should be stored in covered areas or closed cabinets and should never be stored under sinks or next to trash receptacles, where they could come in contact with contaminates or moisture.
The orthodontic assistant can give the patient home care instruction after placement of the TAD. Patients should rinse their mouths with chlorhexidine two to three times per day for the first 7 days. During the first week, patients should also dip their toothbrush in the chlorhexidine and brush around the miniscrew. Thereafter, the patient should brush the TAD as if it were a tooth.
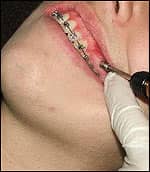 |
| Once identified, a TAD with TAP should be removed. |
TADs and TAP
Make sure to advise patient to tell the orthodontist about any swelling or pain that occurs, as this may be a sign of infection. One of the complications of TAD placement is an infection sometimes called periimplantitis. To label infections involving the bone surrounding TADs as periimplantitis is, in fact, a misnomer. Periimplantitis is defined as the pathologic changes confined to the surrounding hard and soft tissues adjacent to an osseointegrated implant. The diagnosis of periimplantitis is confirmed by a gradual loss of bone around an osseointegrated implant documented via probing depths and serial radiographs. Because no such osseointegration takes place with most TADs, and they are usually removed less than 12 months after initial placement, a term that is more applicable to TADs in orthodontics is needed. For the purposes of this discussion, I will use the term “temporary anchorage periimplantitis,” or TAP, to properly differentiate this phenomenon from true periimplantitis.
Much like periimplantitis, TAP may result from anaerobic bacterial infection at the bone-to-implant interface. Localized bone loss may occur with TAP, resulting in progressive TAD mobility and pain. Radiographic evidence may not be helpful in these situations, given the brief nature of the TAD’s role in an orthodontic treatment plan. Because of this, the clinician must identify the potential existence of TAP by clinical evaluation and move forward with the appropriate treatment.
Once identified, a TAD that has TAP should be removed. Antibiotic therapy generally is not indicated; however, several days of chlorhexidine rinses should be prescribed to help resolve any associated inflammation.2
With the growing use of TADs, surgical procedures are being performed in the orthodontic practice. To reduce risks of infection, the orthodontist and the orthodontic assistants must increase their understanding of basic infection-control practices. This includes training on procedures on how contaminated instruments are cleaned, packaged, sterilized, and stored. According to Graham, orthodontic assistants need to be aware of the fact that placing TADs is very easy for the orthodontist to do, and painless for the patient. Patients may have TADs placed in an open-bay setting, and others in the clinic will have no idea that anything other than a routine orthodontic visit is taking place. Having confidence in their orthodontist and in the TAD system is one of the greatest contributions that an orthodontic assistant can provide to the success of any TAD case.
Leslie Canham, CDA, RDA, is a speaker and consultant specializing in infection control and OSHA compliance. She provides in-office training, mock inspections, and consulting. She can be reached through www.lesliecanham.com or at (888) 853-7543. If you would like a complimentary copy of an OSHA Training Checklist, you may request one by e-mailing /i>.
References
- Kohn, WG, Collins AS, Cleveland JL, Harte JA, Eklund KJ. Guidelines for infection control in dental health-care setting – 2003. www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm. Accessed August 22, 2007.
- Graham JW, Cope JB. Miniscrew Troubleshooting. Orthodontic Products. 2006;13(3):26–32.








