by Michael J. Mayhew, DDS, MS, MS
The possibilities of the paperless, plasterless practice

Michael J. Mayhew
DDS, MS, MS
Like many orthodontists, I welcomed the decision to adopt a computerized practice-management and charting system that made our office “paperless.” Eliminating the physical storage of plaster models, or becoming “plasterless,” was another primary interest for our practice. Approximately 8 years ago, we selected Cadent’s OrthoCAD iCast digital modeling product as our solution for model storage and retrieval. It also provided state-of-the-art diagnostics and the ability to communicate electronically with referring doctors and patients.
My interests soon progressed to assisting OrthoCAD in development and delivery of its iQ product, which uses digital modeling and virtual alignment to help with indirect bonding. iQ uses digital mapping of the patient’s unique dental anatomy, joined with the orthodontist’s prescription plan and bracket of choice, to provide a virtual alignment that demonstrates both bracket expression and alignment capabilities. Virtual alignment also allows users to consider multiple treatment plan options and share these options with both the referring dentist and the patient. We found this particularly useful in planning prerestorative orthodontic cases with referring dentists.
The initial OrthoCAD product proved to have a cumbersome method of transferring the patient’s virtual bracket information from the computer to the patient’s dentition. It used an intraoral camera with a “smart bomb” targeting method to locate the optimal bracket position directly to the patient’s tooth. Once the computer position was matched to the patient’s tooth, the bracket was cured to that location. I experimented using this same intraoral camera and “smart bomb” targeting method to the patient’s plaster model and then used standard techniques to fabricate carrier trays for an indirect bonding process.1,2 Merging the CAD/CAM technology with time-proven indirect bonding techniques proved to be the optimal method to transfer the virtual bracket positioning to the patient. Our experience with the new techniques was described in a publication in 2005.3
Perhaps the most anticipated new technology in our office has been Cadent’s iTero iOC intraoral scanner. It eliminates alginate or PVS impressions and creates a digital model that is more accurate than those created from impressions. We have found that patients experience less anxiety, less gagging, and less discomfort than with other impression techniques. Parents and patients also appreciate that we are using advanced technologies for their orthodontic care.
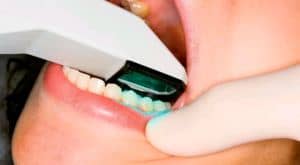
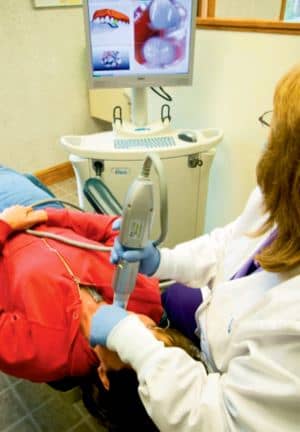
Figure 1: A clinical staff member takes a digital intraoral scan. Full-mouth scan times for the iTero iOC intraoral scanner range from 6 to 10 minutes, depending on the number of teeth to be scanned.
Taking the Scan
Our clinical staff have found the scanner easy to manipulate and the process simple to master, which means fewer retakes (Figure 1). Computer prompts tell the operator what areas to scan, software knits the multiple scans together, and a real-time model can be viewed chairside. Any areas that were not captured fully can be readily rescanned, avoiding a repeat appointment due to a poor impression. A key difference between the iOC scanner and others on the market is that iOC does not require powder. Powdered scanning techniques require clinical staff to hover the scanner over the area to be imaged, whereas the iOC scanner allows for contact scanning. Typical full-mouth scanning times range from 6 to 10 minutes depending on the number of teeth to be scanned. The iOC scanner uses parallel confocal imaging to digitally capture the surface and contours of the teeth and gingival structures. Through a combination of laser and optical scanning, the detector captures 100,000 points of laser light in perfect focus at 300 focal depths of the tooth structures.
Once the scan is complete, cleanup includes disposal of the single-use imaging shield that protects the scanner lens and contacts the patient’s teeth and soft tissues. Surface disinfection of the scanner body held by the clinical staff completes the process.
Our clinical staff appreciate the elimination of impression preparations, the storage of impression trays, cleanup, disinfection of the impressions, pour-up or preparing impressions to be shipped, trimming models, cataloguing, storage, and retrieval. Instead, we get immediate feedback, efficient turnaround time from the lab, and the ability to start cases faster than with other computer-assisted bracket-placement systems. And, of course, we no longer need to purchase impression materials and trays.
From Scan to Mouth
Following completion of the scan and approval by the clinician, the scan file is uploaded to Cadent. The orthodontist has access to the model via myaligntech.com (formerly mycadent.com) and enters an iQ prescription plan online.
Prescription plan options include the type of bracket and wire shape preferred by the orthodontist as well as typical selections relative to the type of alignment and treatment finish desired. Online prescriptions also allow freehand comments so that the orthodontist can interact directly with the OrthoCAD technician. The orthodontist gets an e-mail when the iCast is available for viewing and about virtual alignment cases ready for review and approval (Figure 2).
Interactive software allows the orthodontist to adjust bracket positioning in real time to refine the virtual alignment as desired and make the approval that prompts the iQ tray fabrication (Figures 3 and 4).
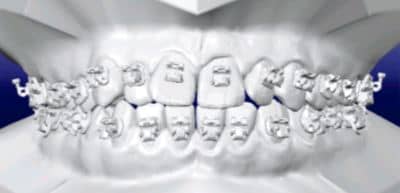
Figure 2: Cadent uses your patient’s impression and prescription to generate a 3D digital model showing optimal bracket placement to achieve the prescribed results.
The iTero scanner operates on an open-architecture platform, allowing the scanner data to be used in multiple ways. Besides the family of products that OrthoCAD provides, the scanner data has potential for compatibility with a range of products that fabricate custom brackets and wires, guide robotic bending of wires, and fabricate orthodontic treatment or retention appliances on printed stereolithic models.
Recently, Align Technologies acquired Cadent and made the iOC scanner an integral part of the impression process for Invisalign. The protocol for aligners currently requires a minor change in the scanner process to obtain more interproximal detail for retentive purposes. This has a small impact on scan times. Using the scans for Invisalign appears to expedite the initial process, shortening the overall time to receive aligners.
Placement and Bonding
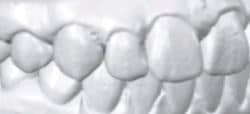


Figures 3A-C: The orthodontist reviews the virtual setup determined by the prescription and bracket selections and, if needed, modifies tooth positions using the OrthoCAD software. Approval of the final setup initiates the tray-fabrication process for indirect bonding.
Studies comparing the accuracy of bracket placement between direct and indirect bonding methods have all found some inaccuracies in one or more alignment variables.4-8 However, direct bonding by itself has been shown to have greater range of angulation, vertical, and mesial-distal errors.8 Digital virtual bracket placement allows the orthodontist to visualize how a specific bracket position will affect tooth movement and create the desired treatment changes. The interactive aspects of the OrthoCAD software allow the orthodontist to modify individual bracket positions and resultant tooth movements, providing an opportunity for multiple setups that can be shared with patients, parents, and referrers.
Once the orthodontist has approved the virtual setup, OrthoCAD technicians use a 3D printed model fabricated from the original scan for bracket placement and bonding tray development. Before they are placed in a dual-tray indirect bonding setup (Figure 5), the brackets are positioned using a “smart bomb” targeting technique that transfers virtual alignment information to the model (Figure 6). The custom bases are then light-cured.
While indirect bracket positioning (and, specifically, virtual alignment visualization) can aid the clinician in correcting a particular malalignment scheme, a specific concern is loss of orientation of the patient’s facial and smile aesthetics. Beyond straightening teeth, optimal bracket positioning should also achieve tooth positioning that complements the dynamics of the patient’s facial and smile aesthetics.9

Figure 4: A customized tray with brackets positioned to achieve your desired treatment outcome is created and shipped to your office, ready for the indirect bonding process.
Currently we satisfy this demand by obtaining multiple measurements of the patient at the initial exam that pertain to both static and dynamic smile aesthetics. A particular positive aspect of a tooth position may then be used as a landmark that is protected so that adjacent bracket positions can be changed to align the remaining dentition to it. If the patient presents with an optimal maxillary incisor display and a deep bite, we try to maintain the maxillary incisor position while employing treatment techniques that open the bite by leveling the lower arch. Likewise, inadequate maxillary incisor display may be improved by more apical positioning of the brackets to erupt incisors and improve smile esthetics. Figure 7 (page 20) demonstrates the virtual placement of brackets more gingivally to erupt the incisors, close the bite, and improve incisor display and the clinical effect noted for the patient early in treatment.
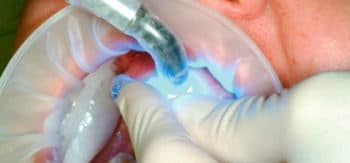
Figure 5: Using indirect bonding techniques to complete full bracket placement.
With this system, we use typical indirect bonding techniques with optimal isolation to maintain a dry and accessible field. We prep the custom composite bases on the brackets with an application of OrthoSolo (from Ormco) or Assure (from Reliance Orthodontics Products). This promotes the bonding medium (Flo-Tain from Reliance Orthodontics Products) to adhere to the custom bases. We apply Flo-Tain to the custom bases along the gingival aspects, seat the trays, and light-cure the composite. We then remove the dual bonding trays and clean up any bonding residue before placing the wires. The total process for bracket application varies from 15 to 20 minutes, with 5 chairside minutes scheduled for the orthodontist for each bonding appointment.
Midtreatment Adjustments
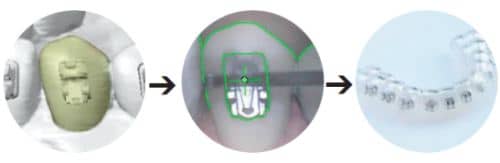
Figure 6: iQ uses a “smart bomb” targeting technique to transfer the virtual alignment information to a model of the patient’s teeth for tray fabrication and preparation for indirect bonding.
During treatment, it is important to continue to evaluate bracket positioning relative to tooth movement. Gingival tissues or severe tooth rotations may not allow optimal virtual bracket positioning. Occasionally, it is best to either bond an eyelet to a rotated tooth or to leave the bracket off the virtual setup and bond directly, possibly with laser gingivectomy procedures to assist with crown exposure. We currently schedule our patients for a panoramic film and repositioning appointment approximately 6 months into treatment or following 8 weeks of treatment with the first rectangular archwire in the Damon System (from Ormco). While you should expect detailing wire adjustments, repositioning brackets is preferable to wire bends if at all possible. The same archwire can typically be replaced after repositioning so that the normal progression of wires can continue at subsequent appointments.
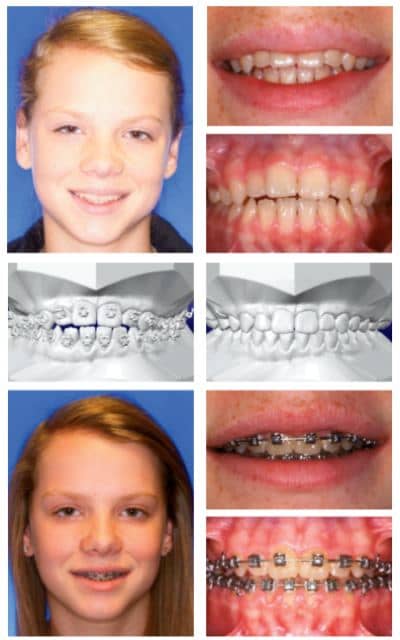
Figure 7: Clinical data merged with virtual alignment is designed to allow for optimal bracket positioning.
Occasionally, we see virtual bracket positioning where we simply are not certain that the tooth will align with the bracket in that position! However, with the detailed mapping of the facial tooth-surface anatomy, a bracket may be virtually positioned differently from one that an orthodontist would have normally direct-bonded the tooth to achieve alignment.
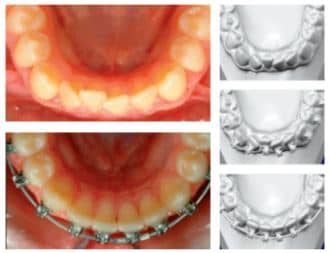
Figure 8: Typical consideration would be a more mesial bracket position for the lower laterals, yet mesial facial position of virtual alignment results in optimal clinical alignment.
Figure 8 shows the malaligned lower lateral incisors where classic positioning with direct bonding may have placed brackets to the distal for optimal alignment, while the virtual setup demonstrates alignment achieved best with a slightly mesial positioning. Tooth-surface mapping provides an improved positioning of a standard bracket to optimize alignment. We have learned to trust those unique bracket positions into a full-dimension wire and then to adapt if necessary to complete the treatment goals.
What’s Next?
Orthodontists have expressed an interest in using CBCT scans to obtain digital models that provide root anatomy information and therefore more detailed virtual alignment potential.10 While controversy exists regarding radiation dosimetry with CBCT use in orthodontics, an additional concern is the ability to obtain adequate tooth-surface detail. A highly detailed intraoral scan of teeth combined with a less detailed CBCT root structure digitally “knitted” to the scanned teeth may prove to be the most radiation-hygienic method of depicting root structures from virtual alignment to optimal clinical results.
While the advent of straight-wire orthodontic appliances placed a premium on bracket positioning, the orthodontist of the future may best serve his patients by becoming the best treatment-planner (assisted by CAD/CAM orthodontics) and also the best clinical case manager of those applied techniques. The iTero intraoral scanner bridges the gap between the patient’s introduction to computerized records and the technologically advanced treatment modalities of today’s modern orthodontic practice.
Michael J. Mayhew, DDS, MS, MS, is board-certified in pediatric dentistry and orthodontics, having received those degrees and his DDS degree at UNC-Chapel Hill. He has a dual-specialty practice in Boone, NC, holds an adjunct professor position at UNC School of Dentistry, and serves on the sports medicine team at Appalachian State University. He lectures for Ormco on self-ligation and serves as an advisor for Cadent OrthoCAD. He can be reached at
References
- Thomas RG. Indirect bonding: Simplicity in action. J Clin Orthod. 1979;13:93-106.
- Hickham JH. Predictable indirect bonding. J Clin Orthod. 1993;27:215-217.
- Mayhew M. Computer-aided bracket placement for indirect bonding. J Clin Orthod. 2005;11:653-660.
- Aguirre MJ, King GJ, Waldron JM. Assessment of bracket placement and bond strength when comparing direct bonding to indirect bonding techniques. Am J Orthod. 1982;82:269-276.
- Koo BC, Chung CH, Vanarsdall RL. Comparison of the accuracy of bracket placement between direct and indirect bonding techniques, Am J Orthod. 1999;116:346-351.
- Taylor NG, Cook PA. The reliability of positioning preadjusted brackets: An in vitro study. Br J Orthod. 1992;19:25-34,1992.
- Balut N, Klapper L, Sandrik J, Bowman D. Variations in bracket placement in the preadjusted orthodontic appliance. Am J Orthod. 1992;102:62-67.
- Hodge TM, Dhopatkar AA, Rock WP, Spary DJ. A randomized clinical trial comparing the accuracy of direct and indirect bracket placement. J Orthod. 2004;31:132-137.
- Sarver D. Soft tissue-based diagnosis and treatment planning. Clinical Impressions. Vol. 14, 1:21-26.
- Guo H, Zhou J, Bai Y, Li S. A three-dimensional setup model with dental roots. J Clin Orthod. 201;44:209-216.










